Table of Contents >> Show >> Hide
- Why ICU Doctors Matter So Much
- What the “Biden Ban” Debate Is Really About
- The ICU Workforce Shortage Is Bigger Than One Policy
- How Tele-ICU Can Help Smaller Hospitals
- Why Medicare Payment Rules Matter
- Patient Safety, Oversight, and the Case for Guardrails
- Rural America Feels the ICU Gap First
- The Pandemic Exposed the Fragility of Critical Care
- What Should Policymakers Do?
- Experiences and Real-World Lessons from the ICU Doctor Gap
- Conclusion
When people hear the phrase “ICU shortage,” they often imagine a hospital hallway packed with beds, beeping machines, and nurses moving so quickly they deserve their own weather system. But one of the most dangerous shortages in American critical care is less visible: the lack of board-certified ICU doctors, also known as intensivists. These are the physicians trained to manage the sickest patients in the hospital, from severe respiratory failure to sepsis, shock, complex infections, and multi-organ failure.
The phrase “Biden ban” has been used by critics to describe a Medicare payment problem affecting some tele-ICU doctors who are licensed and trained in the United States but physically located outside the country while treating patients remotely. It is not the official name of a law or regulation. The real issue is older and more complicated than any campaign slogan: Medicare generally does not pay for medical services furnished outside the United States, and that rule has collided with modern telemedicine in a way that can limit hospital access to remote ICU specialists.
In plain English, the debate comes down to this: if a qualified American ICU doctor is sitting in Canada, Europe, or another country while remotely guiding care for a patient in a U.S. hospital ICU, should Medicare reimburse that care? Critics say yes, because the patient is in America, the hospital is in America, and the doctor may be fully licensed to treat that patient. Federal policy has generally said no, because the service is considered tied to the physician’s location. That is where the controversy begins, and like many healthcare arguments, it comes with enough fine print to make a lawyer’s printer overheat.
Why ICU Doctors Matter So Much
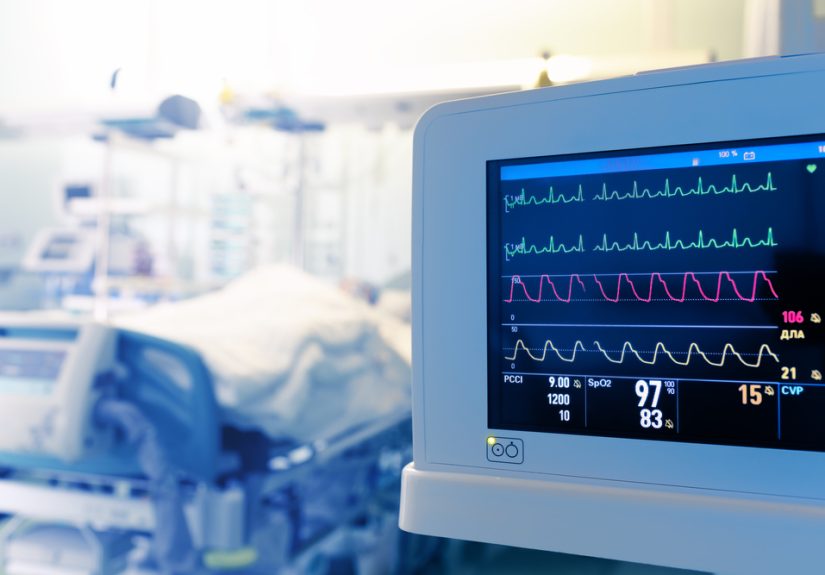
An ICU is not simply a room with extra tubes and dramatic lighting. It is a highly specialized environment where minutes can matter. ICU doctors coordinate ventilator settings, medications that support blood pressure, infection treatment, kidney support, sedation plans, and decisions about whether a patient needs transfer to a higher level of care. They also work with nurses, respiratory therapists, pharmacists, surgeons, hospitalists, and families during some of the most stressful hours of a patient’s life.
Many hospitals, especially smaller rural hospitals, do not have an intensivist physically present around the clock. Some do not have one at all. Instead, they rely on general physicians, hospitalists, emergency physicians, nurse practitioners, physician assistants, and transfer agreements with larger medical centers. Those teams can provide excellent care, but critical illness is a specialty for a reason. A crashing ICU patient is not the ideal moment for “let’s Google that” energy.
Tele-ICU programs were created to help close this gap. Through secure video, electronic health records, remote monitoring, and real-time communication, an off-site intensivist can support bedside teams in multiple hospitals. This does not replace the nurse at the bedside or the local physician who can physically examine the patient. Instead, it adds another brain to the roompreferably one that has spent years learning how to keep very sick people alive.
What the “Biden Ban” Debate Is Really About
The phrase “Biden ban” is politically loaded, but the policy problem is not new. Medicare’s restrictions on payment for care furnished outside the United States come from long-standing federal law. The original purpose was understandable: Medicare was designed to cover care for eligible beneficiaries inside the United States, with only narrow exceptions for certain foreign emergencies. It was not written for a world where a doctor could sit in Vancouver, log into a secure U.S. hospital system, and help manage a ventilator in Louisiana.
That is why the controversy feels like a 1960s rule wearing a 2020s headset. The law was created in an era of paper charts, rotary phones, and televisions that weighed more than a golden retriever. Modern telemedicine has changed what “location” means in healthcare. A physician may be physically outside the country while the patient, hospital, nurses, medical records, medications, and clinical consequences are all inside the United States.
Critics argue that denying reimbursement in these cases makes no clinical sense when the doctor is otherwise qualified, licensed, credentialed, and able to help. Supporters of strict payment rules argue that Medicare has to follow the statute, prevent fraud, maintain oversight, and avoid opening a loophole that could be difficult to regulate. Both concerns are real. The hard part is designing a policy that protects patients without creating a bureaucratic moat around medical expertise.
The ICU Workforce Shortage Is Bigger Than One Policy
Even if the overseas tele-ICU payment issue were fixed tomorrow, America would still face a serious physician workforce challenge. The country has an aging population, rising chronic disease burden, uneven distribution of doctors, and a long training pipeline. Becoming a critical care physician often requires medical school, residency, and fellowship. In other words, you cannot solve the problem by posting “ICU doctor needed ASAP” on a job board and hoping for the best by Tuesday.
National physician-shortage projections show that the U.S. healthcare system is under long-term pressure. Specialty shortages are especially difficult because training takes many years and because specialists tend to concentrate in larger cities and academic hospitals. Rural communities often feel the squeeze first and hardest. When a hospital is small, far from a major medical center, or financially fragile, recruiting a full-time intensivist can be like trying to hire a snowplow driver in Miami: possible, but not easy.
Hospital closures and service-line reductions have also affected ICU capacity. A hospital can have beds on paper but still be unable to safely staff them. ICU capacity depends on trained nurses, respiratory therapists, pharmacists, physicians, equipment, transfer networks, and money. Remove one piece, and the whole machine starts making noises nobody wants to hear.
How Tele-ICU Can Help Smaller Hospitals
Tele-ICU is not science fiction. It is already used in many health systems to extend critical care expertise. In a typical model, a remote command center is staffed by intensivists and critical care nurses who monitor patients across several facilities. They can review vital signs, lab results, imaging, medication changes, and alerts. They can join bedside rounds, help identify early deterioration, recommend changes, and support night coverage when local resources are thin.
For a small hospital, tele-ICU can mean the difference between managing a patient locally and transferring that patient hours away. Transfers are sometimes necessary, but they are not magic carpets. They require ambulance or air transport, available beds, accepting physicians, weather cooperation, and time. During a severe respiratory failure case, time is not a decorative accessory; it is the main character.
Tele-ICU also supports bedside clinicians. Nurses and hospitalists in smaller facilities often carry enormous responsibility. Having a critical care physician available remotely can reduce isolation, improve confidence, and help standardize care. It is not about replacing local teams. It is about giving them backup before a difficult case becomes a tragedy with paperwork.
Why Medicare Payment Rules Matter
Some readers may wonder, “If the doctor can help, why doesn’t the hospital just use the doctor and figure out payment later?” That sounds reasonable until you remember that hospitals are not lemonade stands with stethoscopes. They operate under strict billing rules, payer contracts, compliance systems, staffing budgets, malpractice requirements, and accreditation standards. If Medicare will not reimburse a service, hospitals may be unable or unwilling to build that coverage into their regular ICU staffing model.
Medicare payment policy also influences private insurers and state Medicaid programs. When Medicare draws a line, other payers often pay attention. That means a federal rule can shape what hospitals can afford, what staffing models they use, and whether remote specialist coverage is available in communities that need it most.
The controversy becomes sharper when the physician is not a random doctor in a beach chair trying to practice medicine over hotel Wi-Fi. Critics focus on U.S.-trained, board-certified, credentialed physicians who may be temporarily or permanently located abroad but still able to provide telecritical care to American hospitals. If a doctor can provide safe remote ICU care from Detroit, critics ask, why is the same doctor suddenly unusable from Toronto?
Patient Safety, Oversight, and the Case for Guardrails
Still, any reform would need guardrails. Remote ICU care is high-stakes medicine. Policymakers would need to ensure that physicians are properly licensed in the patient’s state, credentialed by the hospital, covered by malpractice insurance, available for real-time communication, integrated with the local care team, and subject to U.S. quality and privacy standards. Nobody wants “international mystery doctor” as a new hospital staffing category.
There are also legitimate concerns about enforcement. If Medicare allows payment for remote services furnished from outside the country, how does it verify location, qualifications, documentation, and compliance? How does it prevent abuse without blocking legitimate care? These are solvable questions, but they are not tiny questions. In healthcare policy, every loophole eventually attracts someone carrying a billing manual and a suspiciously large invoice.
A reasonable policy path could allow narrow exceptions for tele-ICU services when the patient is in a U.S. hospital, the physician is U.S.-licensed and hospital-credentialed, the service meets Medicare documentation standards, and the hospital maintains responsibility for clinical integration. That would not be a free-for-all. It would be a targeted fix for a targeted workforce problem.
Rural America Feels the ICU Gap First
The ICU doctor shortage is not evenly distributed. Large academic hospitals may have teams of intensivists, fellows, residents, pharmacists, and respiratory therapists. Rural hospitals may have a small staff doing heroic work with fewer resources and a transfer center on speed dial. For patients, geography can become destiny. A heart attack, stroke, septic infection, or severe pneumonia does not politely wait until a specialist is nearby.
Rural patients also tend to be older and may have more chronic conditions. That increases the need for emergency and critical care. Yet these same communities often face physician shortages, hospital financial stress, ambulance delays, and fewer specialty services. Tele-ICU cannot solve all of that, but it can bring expertise into places where recruiting a full-time specialist is unrealistic.
This is why the debate over remote ICU reimbursement matters. It is not just a billing footnote. It affects whether hospitals can assemble coverage models that stretch scarce specialists across more communities. When the supply of intensivists is limited, every qualified hour matters. Wasting available expertise because of geography feels especially painful when the patient’s geography is exactly the problem.
The Pandemic Exposed the Fragility of Critical Care
COVID-19 did not create America’s ICU workforce shortage, but it did slap a spotlight on it. During surges, hospitals learned that beds are not truly beds unless trained staff are available to care for the person in them. Ventilators matter, but ventilators do not run themselves. ICU nurses, respiratory therapists, and physicians became the limiting resource.
The pandemic also accelerated telehealth adoption. Many patients discovered that a video visit could save time, reduce travel, and increase access. Hospitals expanded remote monitoring. Regulators temporarily loosened some telehealth rules. The healthcare system learned, under pressure, that not every useful medical interaction requires two humans to be in the same room. Unfortunately, payment policy did not evolve evenly across every setting and scenario.
Tele-ICU sits at the intersection of these lessons. It is remote care, but not casual care. It is technology-enabled, but deeply clinical. It can expand access, but only if payment policy, licensing, hospital credentialing, and quality oversight line up. When they do not, the result is predictable: patients need care, doctors are available, hospitals are interested, and the rulebook says, “Please hold while we transfer your crisis to 1965.”
What Should Policymakers Do?
1. Create a Narrow Medicare Exception for Qualified Tele-ICU Care
Congress or regulators could explore a carefully defined exception for critical care telehealth provided to patients located in U.S. hospitals by U.S.-licensed, board-certified physicians outside the country. The exception should be narrow, audited, and tied to hospital credentialing and quality reporting. The goal would not be outsourcing American medicine. The goal would be preventing avoidable gaps in ICU expertise.
2. Expand the Critical Care Workforce Pipeline
Tele-ICU is a bridge, not a factory. America still needs more physicians, nurses, respiratory therapists, and advanced practice clinicians trained in critical care. That means expanding residency and fellowship capacity, supporting rural training tracks, reducing burnout, improving working conditions, and making critical care careers sustainable. A burned-out intensivist is not a renewable resource.
3. Invest in Rural Telehealth Infrastructure
Remote critical care depends on reliable broadband, secure platforms, interoperable electronic records, trained bedside teams, and clear protocols. A tele-ICU connection that freezes during an emergency is not innovation; it is a very expensive buffering symbol. Rural hospitals need technical and financial support to make tele-ICU practical.
4. Protect Quality While Expanding Access
Any reform must include safeguards: state licensure, malpractice coverage, real-time availability, documentation standards, privacy protections, hospital oversight, and outcome measurement. Patients deserve access, but they also deserve accountability. A smart policy can provide both.
Experiences and Real-World Lessons from the ICU Doctor Gap
Imagine a small community hospital on a winter night. The emergency department is already full. A patient arrives with severe pneumonia, low oxygen levels, and blood pressure dropping faster than everyone’s mood. The local physician stabilizes the patient, the nurses start medications, respiratory therapy adjusts oxygen support, and the team tries to transfer the patient to a larger hospital. The transfer center says there are no beds. Another hospital says call back later. A third asks for more labs. Meanwhile, the patient is not interested in administrative suspense.
This is where tele-ICU can become more than a technology pitch. A remote intensivist can review the case, help adjust ventilator settings, recommend vasopressors, guide antibiotic choices, and help the local team decide whether the patient can stay safely or must be transferred at all costs. For families, that may mean their loved one receives specialist input without being moved far from home. For clinicians, it may mean having a calm expert voice during a chaotic hour.
There is also an emotional side that rarely appears in policy documents. Families often assume that “ICU” automatically means an ICU doctor is present. That is not always true. In many hospitals, especially at night, the bedside team may be excellent but stretched thin. A family member may see monitors, IV pumps, and a glass-walled room and believe every possible specialist is involved. In reality, the hospital may be doing its best with limited personnel. The gap between expectation and staffing reality can be heartbreaking.
Clinicians feel this too. Nurses in under-resourced ICUs often carry the moral weight of knowing a patient needs more help than the facility can provide. Hospitalists may manage critical illness outside their deepest specialty because there is no one else. Emergency physicians may board ICU patients for hours while waiting for beds. These professionals are not failing; they are absorbing system failure at bedside speed.
The overseas tele-ICU payment controversy adds another frustrating layer. When a qualified doctor is available remotely but payment rules make using that doctor financially risky, the system creates an artificial shortage on top of a real shortage. It is like being thirsty, seeing a water fountain, and being told the plumbing is technically located in the wrong ZIP code.
Patients do not care whether the expert helping them is ten miles away or across a border if the care is safe, legal, secure, and effective. They care whether someone recognizes deterioration early. They care whether the ventilator settings are right. They care whether their parent, spouse, sibling, or child has the best possible chance. Policy should care about that too.
The most practical lesson is that healthcare access is not only about insurance cards or hospital buildings. It is about whether the right person can deliver the right expertise at the right moment. ICU care is a team sport, and the scoreboard is brutally honest. When America has too few intensivists, every sensible tool should be on the table: better training pipelines, smarter staffing models, rural support, tele-ICU expansion, and payment rules that reflect modern medicine rather than yesterday’s map.
Conclusion
The claim that millions of Americans are without ICU doctors because of the “Biden ban” is best understood as a political shorthand for a narrower but very real policy dispute. The core issue is not that one administration invented a simple ban. It is that long-standing Medicare rules on services furnished outside the United States have collided with tele-ICU medicine at a time when America already faces serious physician shortages.
The solution is not to throw away oversight or pretend geography never matters. The solution is to modernize payment rules carefully, expand the critical care workforce, support rural hospitals, and use telemedicine where it can safely extend specialist expertise. In the ICU, the best policy is the one that helps qualified clinicians reach patients before the crisis wins.