Table of Contents >> Show >> Hide
Diabetes is one of those health topics that sounds simple until you actually try to explain it at the dinner table. “It has something to do with sugar,” someone says, while another person bravely pushes the dessert plate away like it just insulted their ancestors. In reality, diabetes is not just about eating sweets, and it is definitely not a personal failure wrapped in a blood test result. It is a group of conditions that affect how the body uses glucose, the main fuel that keeps your cells powered, your brain thinking, and your feet moving toward the refrigerator at midnight.
When diabetes is managed well, people can live active, full, and very normal lives. When it is ignored, however, high blood sugar can quietly damage the heart, kidneys, nerves, eyes, blood vessels, and more. That is why understanding diabetes symptoms, causes, treatment options, and prevention strategies matters. The earlier you recognize the signs and build healthy routines, the better your chances of staying ahead of complications.
This guide breaks down diabetes in plain English: what it is, how it feels, why it happens, how doctors diagnose it, how it is treated, and what you can do every day to lower risk. No panic. No blame. Just useful information with a little humor, because the pancreas may be serious, but your article does not have to be boring.
What Is Diabetes?
Diabetes is a chronic condition in which blood glucose, often called blood sugar, becomes too high. Glucose comes from the foods and drinks you consume, especially carbohydrates. After digestion, glucose enters the bloodstream. Insulin, a hormone made by the pancreas, helps move that glucose from the blood into the body’s cells, where it can be used for energy.
In diabetes, this system does not work properly. The body may not make enough insulin, may not use insulin well, or may stop producing insulin almost entirely. As a result, glucose stays in the bloodstream instead of entering cells efficiently. Think of insulin as the key that opens the cell door. In diabetes, the key may be missing, bent, or ignored by the lock.
Main Types of Diabetes
Type 1 Diabetes
Type 1 diabetes is an autoimmune condition. The immune system mistakenly attacks insulin-producing cells in the pancreas. Because the body makes little or no insulin, people with type 1 diabetes need insulin treatment to survive. It often begins in childhood or adolescence, but adults can develop it too. Type 1 diabetes is not caused by eating too much sugar, being lazy, or forgetting to own a yoga mat.
Type 2 Diabetes
Type 2 diabetes is the most common form. It usually begins with insulin resistance, meaning the body’s cells do not respond well to insulin. At first, the pancreas may produce extra insulin to compensate. Over time, it may not keep up, and blood sugar rises. Type 2 diabetes is linked to several risk factors, including genetics, excess body weight, inactivity, age, prediabetes, a history of gestational diabetes, and certain health conditions such as high blood pressure.
Gestational Diabetes
Gestational diabetes develops during pregnancy. It often has no obvious symptoms, which is why screening during pregnancy is important. Many people with gestational diabetes deliver healthy babies, especially with good medical care and blood sugar management. However, it can increase the risk of complications during pregnancy and raise the future risk of type 2 diabetes for both parent and child.
Prediabetes
Prediabetes means blood sugar is higher than normal but not yet high enough for a diabetes diagnosis. It is a warning light on the dashboard, not a life sentence. The good news is that lifestyle changes, especially weight management, regular physical activity, and healthier eating patterns, can often delay or prevent type 2 diabetes.
Common Diabetes Symptoms
Diabetes symptoms can be dramatic, subtle, or sneaky enough to deserve their own spy movie. Some people have obvious symptoms. Others feel completely fine and discover high blood sugar during routine lab work.
Classic Signs of Diabetes
- Frequent urination, especially at night
- Unusual thirst
- Increased hunger
- Fatigue or low energy
- Blurred vision
- Unexplained weight loss
- Slow-healing cuts or sores
- Frequent infections
- Numbness, tingling, or burning in the hands or feet
- Dry or itchy skin
Type 1 diabetes symptoms may develop quickly over days, weeks, or months. Type 2 diabetes symptoms often develop slowly over years and can be so mild that they are easy to overlook. Gestational diabetes usually has no symptoms, which makes prenatal testing especially important.
Why Diabetes Causes Thirst and Frequent Urination
When blood sugar gets too high, the kidneys work harder to remove excess glucose through urine. That extra fluid loss can make you urinate more and feel very thirsty. If you find yourself visiting the bathroom like it is a subscription service, it is worth talking with a healthcare professional.
What Causes Diabetes?
There is no single cause of diabetes. The “why” depends on the type. Type 1 diabetes involves an autoimmune attack and may be influenced by genetics and environmental triggers. Type 2 diabetes develops from a mix of insulin resistance, genetics, lifestyle factors, body weight, age, and metabolic health. Gestational diabetes is connected to hormonal changes during pregnancy that can make insulin less effective.
Risk Factors for Type 2 Diabetes
Type 2 diabetes risk increases with age, family history, physical inactivity, overweight or obesity, high blood pressure, abnormal cholesterol levels, prediabetes, and a history of gestational diabetes. Risk also varies among populations, with higher rates seen in some African American, Hispanic or Latino, American Indian, Asian American, and Pacific Islander communities. These differences are not just about biology; access to healthcare, nutritious food, safe places to exercise, stress, and other social factors matter too.
It is important to say this clearly: diabetes is not a character flaw. Health is shaped by genes, environment, habits, income, sleep, stress, medical care, food access, and a thousand tiny daily realities. Blame is useless. Action is useful.
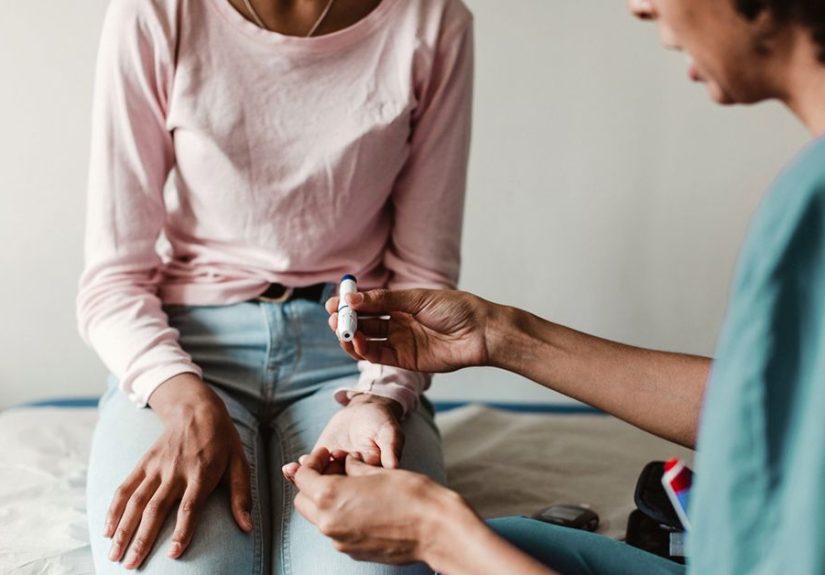
How Diabetes Is Diagnosed
Doctors diagnose diabetes with blood tests. The most common tests include fasting blood glucose, A1C, random plasma glucose, and oral glucose tolerance testing. The A1C test estimates average blood sugar over roughly the past two to three months. It is a helpful tool because it gives a bigger-picture view than one single finger-stick reading after a suspiciously enthusiastic pancake breakfast.
Screening is especially important for people with risk factors. U.S. preventive guidance recommends screening many adults ages 35 to 70 who have overweight or obesity, even when they do not have symptoms. Younger people may also need testing if they have risk factors. Pregnant people are usually screened for gestational diabetes between 24 and 28 weeks of pregnancy, though earlier testing may be needed for those at higher risk.
Diabetes Treatment Options
Treatment depends on the type of diabetes, blood sugar levels, overall health, personal goals, other medical conditions, cost, and daily life. A great diabetes plan should fit the person, not the other way around. Nobody wants a plan that only works if you live inside a wellness brochure.
Healthy Eating
There is no single “diabetes diet” that works for everyone. A balanced plan usually focuses on vegetables, fruits, whole grains, beans, lentils, lean proteins, nuts, seeds, healthy fats, and fewer highly processed foods and sugary drinks. Carbohydrates matter because they affect blood sugar, but that does not mean carbs are villains wearing tiny capes. The type, amount, and timing of carbohydrates are what count.
For example, oatmeal with nuts and berries usually affects the body differently than a large sweetened drink and a pastry. Both may contain carbohydrates, but one brings fiber and nutrients; the other brings a sugar rush and a crash worthy of a movie trailer.
Physical Activity
Regular movement helps the body use insulin better and lowers blood sugar. Many adults aim for at least 150 minutes of moderate-intensity aerobic activity per week, such as brisk walking, cycling, swimming, dancing, or gardening with heroic commitment. Strength training also helps because muscle uses glucose. Even short walks after meals can support blood sugar control.
Medications
People with type 1 diabetes need insulin. People with type 2 diabetes may use lifestyle changes, oral medications, injectable medications, insulin, or a combination. Common medication approaches may include metformin, GLP-1 receptor agonists, SGLT2 inhibitors, DPP-4 inhibitors, sulfonylureas, thiazolidinediones, and insulin. The best choice depends on the individual, especially heart health, kidney function, weight goals, side effects, and affordability.
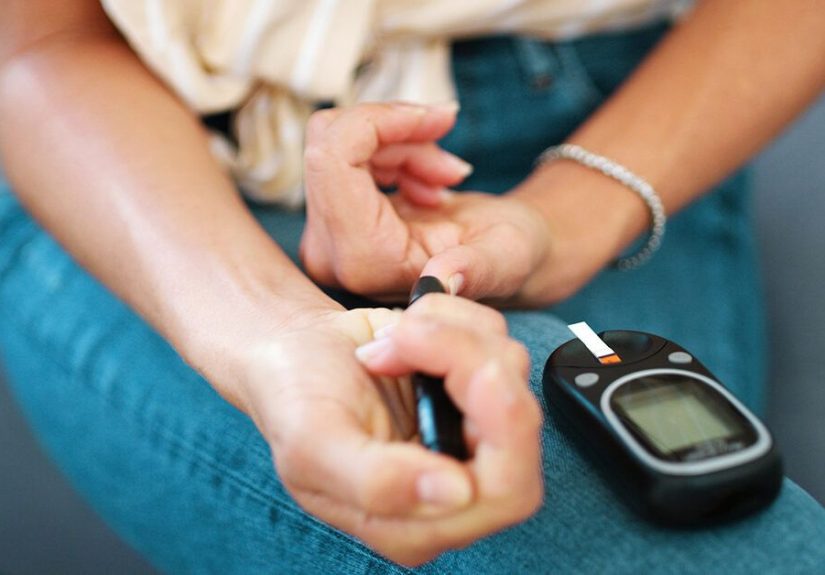
Blood Sugar Monitoring
Some people check blood sugar with a finger-stick meter. Others use continuous glucose monitors, also called CGMs, which track glucose patterns throughout the day and night. Monitoring can reveal how meals, exercise, sleep, stress, illness, and medication affect blood sugar. It turns diabetes management from guesswork into data, which is helpful because the human body does not always send polite calendar invitations before changing its glucose levels.
Regular Medical Checkups
Diabetes care is bigger than blood sugar. It often includes blood pressure management, cholesterol care, kidney testing, eye exams, dental care, foot checks, vaccinations, and mental health support. Diabetes can be demanding, and burnout is real. A strong care team may include a primary care clinician, endocrinologist, diabetes educator, dietitian, pharmacist, eye doctor, dentist, podiatrist, and supportive family members who do not act like the food police.
Possible Diabetes Complications
Long-term high blood sugar can damage blood vessels and nerves. Possible complications include heart disease, stroke, kidney disease, vision problems, nerve damage, foot ulcers, infections, gum disease, and sexual health concerns. The goal of treatment is not to scare anyone; it is to prevent problems before they become major events.
Heart health deserves special attention. Diabetes raises the risk of cardiovascular disease, which is why blood pressure, cholesterol, smoking status, physical activity, and nutrition are major parts of care. Managing diabetes well is not just about “good numbers.” It is about protecting the organs you would very much like to keep using.
Can Diabetes Be Prevented?
Type 1 diabetes cannot currently be prevented. Gestational diabetes risk may be lowered in some people with healthy lifestyle habits before and during pregnancy, though not every case is avoidable. Type 2 diabetes, however, can often be delayed or prevented, especially when prediabetes is identified early.
Practical Ways to Lower Type 2 Diabetes Risk
- Lose a modest amount of weight if you have overweight and your healthcare professional recommends it.
- Move regularly, aiming for consistency rather than perfection.
- Choose water more often than sugary drinks.
- Build meals around fiber-rich foods such as vegetables, beans, lentils, fruit, and whole grains.
- Limit highly processed foods, large portions of refined carbohydrates, and frequent sweets.
- Get enough sleep and treat sleep problems when possible.
- Stop smoking or avoid starting.
- Manage blood pressure, cholesterol, and stress.
- Ask about screening if you have risk factors.
Small changes matter. A 10-minute walk after dinner is not glamorous, but your cells do not require glamour. They appreciate repetition. The best prevention plan is the one you can keep doing when life gets messy, busy, rainy, and full of leftover pizza.
Living With Diabetes: Real-World Experiences and Lessons
Living with diabetes is not just a medical routine; it is a daily relationship with food, movement, emotions, schedules, technology, and the occasional surprise blood sugar number that makes you stare at your meter like it personally betrayed you. Many people describe the early stage after diagnosis as overwhelming. There are new words to learn, new appointments to attend, new labels to read, and new habits to build. It can feel like being handed a manual for a machine you did not know you owned.
One common experience is the “food confusion phase.” A person may hear that carbohydrates raise blood sugar and suddenly look at bread, rice, pasta, fruit, and potatoes as if they are all plotting together. Over time, most people learn that diabetes-friendly eating is not about banning every enjoyable food. It is about portions, pairing, timing, and patterns. For example, eating rice with vegetables, protein, and healthy fat may lead to a steadier glucose response than eating a large bowl of rice by itself. A birthday cupcake is not the end of civilization. It is simply something to plan around, enjoy mindfully, and not invite to breakfast every morning.
Another real-life lesson is that exercise works, but it does not have to look like a dramatic fitness montage. People often discover that walking after meals, taking stairs, stretching during TV time, or doing light strength exercises at home can improve energy and blood sugar patterns. The magic is not in punishing workouts. The magic is in making movement ordinary. Diabetes loves routine; it is less impressed by one heroic workout followed by three weeks of couch diplomacy.
Monitoring can also change how people understand their bodies. A glucose meter or CGM may show that stress, poor sleep, illness, or skipping breakfast affects blood sugar just as much as food. This can be oddly comforting because it proves that numbers are information, not moral grades. A high reading does not mean someone “failed.” It means something needs attention: medication timing, meal balance, hydration, sleep, stress, infection, or a conversation with the healthcare team.
Family and social situations can be tricky. Some people receive too much advice from relatives who suddenly become amateur endocrinologists after reading one headline. Others feel embarrassed checking glucose or taking medication in public. With time, many people become more confident saying, “This is what I need to do for my health.” Supportive friends learn not to pressure, tease, or police. A good support system asks, “How can I help?” not “Are you allowed to eat that?”
The emotional side matters too. Diabetes can be tiring because it asks for attention every day. People may feel frustrated, anxious, guilty, or burned out. That is normal, and it is worth discussing with a clinician, diabetes educator, counselor, or support group. Strong diabetes care includes mental health because humans are not spreadsheets with sneakers.
Many people eventually find a rhythm. They learn their go-to meals, favorite walking routes, medication schedule, appointment routine, and personal warning signs. They learn that progress is not always perfect. A better A1C, fewer glucose spikes, improved blood pressure, more energy, or simply feeling more in control are all wins. Diabetes management is not about becoming flawless. It is about becoming informed, consistent, and kind to yourself while doing the next helpful thing.
Conclusion
Diabetes is serious, but it is also manageable. Understanding the symptoms, causes, treatments, and prevention strategies gives you power. Whether the goal is preventing type 2 diabetes, managing a new diagnosis, supporting someone you love, or simply making sense of your lab results, the best first step is knowledge followed by practical action.
Watch for symptoms such as unusual thirst, frequent urination, fatigue, blurry vision, slow-healing sores, and unexplained weight loss. Know your risk factors. Get screened when appropriate. Work with healthcare professionals to build a plan that fits your body and your life. Eat in a way that supports steady energy, move regularly, take medications as prescribed, monitor when recommended, and protect your heart, kidneys, eyes, nerves, and feet.
Note: This article is for general education and should not replace professional medical advice. Anyone with symptoms of diabetes, very high or very low blood sugar, pregnancy-related concerns, or questions about medication should contact a qualified healthcare professional.