Table of Contents >> Show >> Hide
Your tongue is basically the overworked multitool of your mouth. It helps you taste food, shape words, chew, swallow, and occasionally announce that salsa was a terrible idea. So when something looks odd, feels sore, or suddenly tastes like a handful of pennies, it gets your attention fast.
The tricky part is that “tongue problems” is a big umbrella. Some issues are harmless and temporary, like a minor burn from pizza that was clearly hotter than the surface of the sun. Others point to irritation, infection, dry mouth, nutrient deficiencies, immune problems, or, in more serious cases, precancerous or cancerous changes. The good news is that many tongue conditions can be recognized early and treated effectively once the cause is identified.
This guide breaks down the symptoms to watch for, the most common causes, how doctors and dentists diagnose tongue problems, and what treatment usually looks like in real life.
Common Symptoms of Tongue Problems
Tongue symptoms do not all look the same. Some announce themselves loudly with pain and burning. Others are sneaky and show up only as color changes, texture shifts, or a stubborn patch that refuses to leave.
Pain, burning, or soreness
A sore tongue can happen after a burn, accidental bite, mouth ulcer, infection, dry mouth, or inflammation. Some people describe a stinging or scalding feeling even when the tongue looks completely normal, which can happen with burning mouth syndrome.
Color changes
A healthy tongue is usually pink with tiny bumps called papillae. If the tongue turns white, red, yellow, dark brown, or black, that can signal debris buildup, irritation, infection, inflammation, nutritional deficiency, or another underlying condition. A white coating may be harmless, but a white patch that does not wipe off deserves attention.
Texture changes
The tongue may look smooth, cracked, patchy, swollen, or even “hairy.” Geographic tongue can create map-like red areas with lighter borders. Black hairy tongue can make the surface look fuzzy or stained. A smooth, glossy tongue may appear when papillae are lost, sometimes because of glossitis or a deficiency such as low iron, folate, or vitamin B12.
Swelling
A swollen tongue may cause trouble speaking, chewing, or swallowing. Mild swelling can happen with irritation or inflammation. Severe swelling is more urgent, especially if breathing feels difficult.
Taste changes or dry mouth
If food suddenly tastes dull, metallic, bitter, or just plain wrong, the tongue may not be the only issue. Taste changes can happen with infections, medication side effects, dry mouth, nerve problems, or burning mouth syndrome.
Ulcers, sores, patches, or lumps
Canker sores and traumatic ulcers often heal on their own. But a sore, lump, thickened area, or red or white patch that lasts longer than two weeks should be checked by a dentist or doctor. That is especially important if it bleeds, hurts, causes numbness, or makes swallowing harder.
What Causes Tongue Problems?
The tongue is exposed to everything: heat, friction, bacteria, yeast, medications, dehydration, stress, dental appliances, and whatever “extra hot” seasoning level you regretted five minutes later. That is why tongue problems have a long list of causes.
1. Irritation and trauma
Simple irritation is one of the most common reasons a tongue feels off. Hot foods and drinks can burn it. Sharp teeth, braces, grinding, tongue biting, or poorly fitting dentures can cause soreness, ulcers, and swelling. Tobacco and heavy alcohol use can also irritate oral tissues and raise the risk of more serious disease over time.
2. Infections
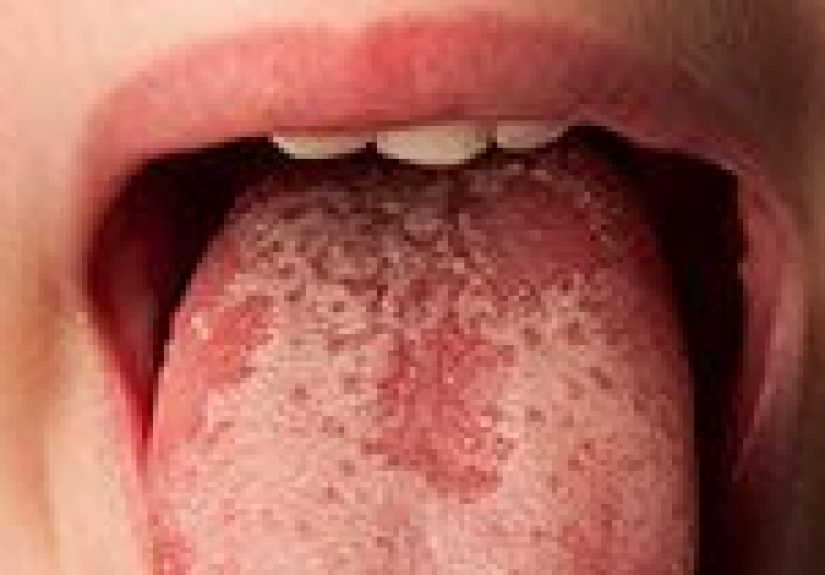
Oral thrush is a yeast infection caused by an overgrowth of Candida. It often causes creamy white patches, redness, soreness, a cottony feeling, and sometimes trouble swallowing. Thrush is more likely after antibiotics, inhaled steroids, dry mouth, diabetes, immune suppression, or certain cancer treatments.
Other infections can also affect the tongue, including viral infections that trigger painful sores or blisters. If a tongue problem appears alongside fever, swollen glands, or widespread mouth pain, infection moves higher on the suspect list.
3. Inflammatory and benign tongue conditions
Some tongue problems look dramatic but are actually harmless. Geographic tongue is a classic example. It causes smooth, red patches that may shift location over time, like a tiny road map that refuses to sit still. It is not contagious and often needs no treatment unless it becomes sensitive.
Black hairy tongue is another startling but usually harmless condition. The papillae get longer than usual and trap debris, bacteria, yeast, tobacco residue, or pigment from foods and drinks. The result can be black, brown, yellow, or green discoloration with a fuzzy appearance.
Oral lichen planus is a chronic inflammatory condition that can affect the mouth and sometimes the tongue. It may cause white, lacy areas, red irritated tissue, or painful erosions.
4. Glossitis and nutritional deficiencies
Glossitis means inflammation of the tongue. It can make the tongue swollen, tender, red, and smooth. Causes include infections, irritants, allergies, and deficiencies in iron, folate, vitamin B12, or other nutrients. Sometimes the tongue becomes one of the first places the body waves a little red flag about a bigger nutritional problem.
5. Dry mouth and systemic conditions
Saliva matters more than most people realize. It protects tissues, helps control bacteria, supports taste, and keeps the mouth comfortable. When saliva drops, the tongue can become dry, rough, cracked, sore, and more prone to infection.
Dry mouth can be linked to medications, dehydration, radiation therapy, diabetes, thyroid disease, and autoimmune conditions such as Sjögren’s disease. In Sjögren’s, dry mouth and dry eyes are especially common, and chewing or swallowing may become uncomfortable.
6. Burning mouth syndrome
Burning mouth syndrome causes burning, tingling, numbness, or scalded sensations, often on the tongue, even when the mouth looks normal. It may occur with dry mouth or altered taste. In some cases, it is secondary to another issue such as nutritional deficiency, reflux, infection, medication effects, hormonal changes, or dry mouth. In other cases, it appears to be related to nerve dysfunction.
7. Precancerous and cancerous changes
This is the category nobody wants, but it is important. Leukoplakia can cause white patches that do not rub off. Some forms are benign, but some can become cancerous, especially when patches are on the tongue or floor of the mouth. Oral hairy leukoplakia is different; it is often linked to Epstein-Barr virus and weakened immunity, particularly HIV, and usually appears as white folded patches on the tongue.
Tongue cancer may cause a nonhealing sore, a lump, persistent red or white patch, bleeding, numbness, pain, trouble swallowing, ear pain, or swollen lymph nodes in the neck. Tobacco, alcohol, and certain HPV-related cancers are major risk factors.
Specific Tongue Problems to Know
Geographic tongue
This harmless inflammatory condition causes smooth red patches with lighter borders. It may move around and sometimes becomes sensitive to spicy, acidic, or hot foods. Many people need no treatment at all.
Glossitis
Glossitis often causes redness, swelling, and a smooth shiny surface. Treatment focuses on the cause, which may include improved oral hygiene, medication for infection, or supplements for nutritional deficiencies.
Oral thrush
Thrush often creates creamy white patches on the tongue and inner cheeks. It is typically treated with antifungal medication, while the underlying trigger, such as inhaler use, immune suppression, diabetes, or dry mouth, should also be addressed.
Black hairy tongue
Despite the dramatic name, this condition is usually temporary and harmless. Better oral hygiene, gentle tongue cleaning, smoking cessation, and reviewing possible medication triggers often help clear it up.
Burning mouth syndrome
This condition can be frustrating because the pain is real even when the tongue looks normal. Treatment may involve correcting an underlying cause, using saliva substitutes, numbing rinses, and, in selected cases, prescription medicines aimed at nerve pain.
Leukoplakia and suspicious patches
If you have a white or mixed red-and-white patch that does not go away, do not ignore it. These lesions often need professional evaluation, and a biopsy may be required to rule out precancer or cancer.
How Tongue Problems Are Diagnosed
Diagnosis starts with the basics: what changed, when it started, what it feels like, and what else is going on. Your dentist or doctor will usually ask about pain, taste changes, dry mouth, smoking, alcohol, medications, recent illness, immune problems, nutrition, and dental appliances.
Next comes the exam. The tongue itself matters, but so do the lips, cheeks, gums, throat, neck, and lymph nodes. Sometimes a careful oral exam is enough to identify a harmless condition like geographic tongue or black hairy tongue.
When the cause is less obvious, testing may include:
- Blood tests to look for anemia, low iron, folate, vitamin B12 deficiency, diabetes, or other systemic problems.
- Evaluation for dry mouth or salivary gland issues.
- A biopsy of a suspicious patch, lump, or lesion.
- Imaging or endoscopy if tongue cancer or a deeper head-and-neck problem is suspected.
If the tongue is severely swollen or you are having trouble breathing, speaking, or swallowing, that is no longer a “wait and see” moment. That is urgent care territory.
Treatment Options for Tongue Problems
Treatment depends entirely on the cause. There is no one magic fix for every sore, coated, burning, swollen, or weird-looking tongue. If there were, it would probably taste terrible.
At-home care for mild irritation
For mild burns, irritation, or temporary soreness, home care may include avoiding spicy or acidic foods, drinking plenty of water, choosing bland foods for a few days, and using gentle oral hygiene. Do not attack your tongue with aggressive brushing like it personally offended you.
Professional dental care
If a rough tooth edge, grinding, poor oral hygiene, or ill-fitting dentures are involved, fixing the dental issue is part of the treatment. Otherwise, the tongue may keep getting re-irritated.
Medications
Doctors may prescribe antifungals for thrush, antibiotics for certain infections, corticosteroid rinses or ointments for inflammatory conditions, or targeted medications for pain relief in burning mouth syndrome. If a nutritional deficiency is the driver, supplements and diet changes are often key.
Managing dry mouth
Treatment may include reviewing medications, treating an underlying condition, increasing hydration, using saliva substitutes, and protecting oral tissues with good dental care.
Treatment for suspicious lesions or cancer
Precancerous or cancerous lesions may require biopsy, removal, and follow-up monitoring. Tongue cancer treatment can include surgery, radiation therapy, chemotherapy, immunotherapy, or a combination, depending on the stage and location.
When to See a Doctor or Dentist
Make an appointment if you have:
- A sore, lump, or patch on the tongue that lasts more than two weeks.
- Persistent white or red patches.
- Ongoing burning, pain, or swelling.
- Trouble swallowing, chewing, or moving the tongue.
- Taste changes that do not improve.
- Repeated thrush, especially if you also have dry mouth or immune issues.
- Unexplained bleeding, numbness, weight loss, ear pain, or a neck lump.
Get urgent care right away if tongue swelling affects breathing.
What Tongue Problems Often Feel Like in Real Life
In real life, tongue problems rarely begin with a dramatic movie soundtrack and a giant neon arrow pointing to the diagnosis. They usually start small. A person wakes up with a sore spot on the side of the tongue and assumes they bit it in their sleep. Another notices a white coating after a round of antibiotics and blames coffee, dehydration, or bad luck. Someone else thinks they burned their mouth on soup, but the soreness keeps returning long after the soup has been forgotten.
One of the most common experiences is confusion. Tongue symptoms can look alarming even when they are harmless, and they can look almost normal when the discomfort is intense. Geographic tongue is a perfect example. People often discover patchy red areas in the mirror and immediately jump to worst-case scenarios. Then the patches move, change shape, or fade, which somehow feels both reassuring and slightly rude. The experience is odd because the tongue can look dramatic but be completely benign, with irritation showing up mostly when spicy salsa, citrus, or hot coffee enters the scene like an uninvited guest.
Burning mouth syndrome creates a different kind of frustration. People often describe it as feeling as though they drank something scalding, except they did not. The tongue may burn in the afternoon, feel metallic by evening, and seem almost normal by breakfast. That pattern can make people feel dismissed because the pain is real, yet there may be no obvious sore, patch, or swelling during an exam. Many spend weeks trying different toothpastes, mouthwashes, and foods before realizing the problem may involve dry mouth, nerve-related pain, medications, reflux, or vitamin deficiencies rather than a visible lesion.
Then there is thrush, which often feels less mysterious and more irritating. People may notice a cottony mouth, odd taste, tenderness, or white patches that make eating less fun than it should be. This can happen after antibiotics, steroid inhalers, or during periods of illness or immune suppression. The experience is often a mix of discomfort and surprise. Many adults assume thrush is something that only happens to babies, then suddenly find themselves googling their tongue in terrible bathroom lighting at 11:47 p.m.
For people with glossitis or deficiency-related tongue changes, the tongue may become smooth, red, and tender. Spicy foods sting. Crunchy foods annoy. Even brushing can feel unpleasant. In some cases, the tongue becomes the clue that leads to a bigger diagnosis such as anemia, low folate, or vitamin B12 deficiency. That is one reason persistent tongue changes should not be brushed off as “just one of those things.” Sometimes the mouth is the first place the body leaves a note.
The most serious real-life experience is the stubborn lesion that does not heal. A patch that sticks around for weeks, a sore that bleeds, or a lump that slowly becomes more noticeable is different from a temporary irritation. People often delay care because the lesion does not hurt much, and that is exactly why regular dental exams matter. Early evaluation can turn a worrying symptom into either peace of mind or a diagnosis caught soon enough to treat more effectively.
Final Thoughts
Most tongue problems are treatable, and many are harmless. But the tongue is also a surprisingly useful messenger. It can reflect irritation, infection, dry mouth, inflammation, nutrient deficiencies, immune issues, and, sometimes, early signs of oral cancer. The smartest move is not panic. It is pattern recognition.
If your tongue changes after a burn, a cold, a new medication, or a rough dental edge, there may be a simple explanation. If the problem lingers, worsens, or comes with red-flag symptoms like a nonhealing sore, persistent patch, or swelling, get it checked. Your tongue does a lot for you every day. Returning the favor with prompt care is a pretty good deal.




