Table of Contents >> Show >> Hide
- Why the 0 to 10 pain scale feels broken
- What a better pain measure should actually include
- The better alternative: measure pain, interference, and function together
- Why this matters for patients, clinicians, and treatment decisions
- How clinics can replace the old scale without making visits longer
- What patients can say instead of “It’s a 7”
- Experiences from real-world pain conversations
- Conclusion
- SEO Tags
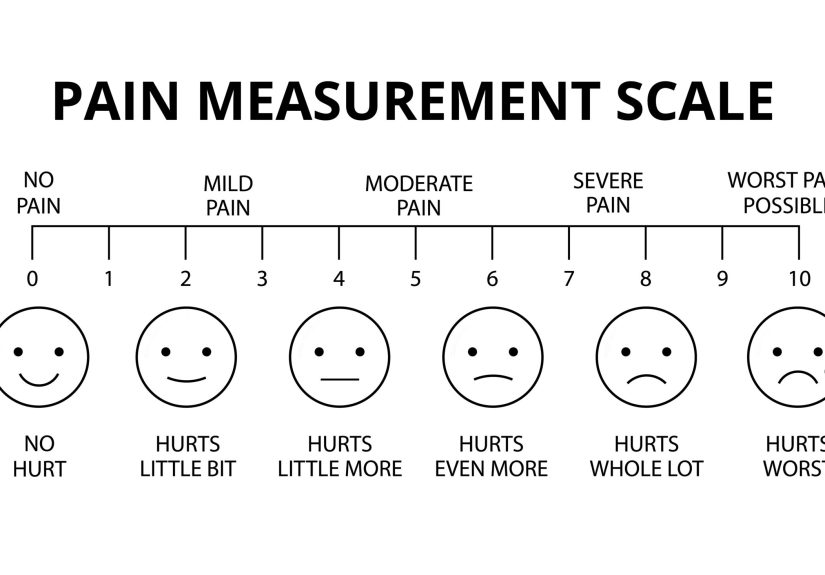
Nearly everyone has heard the question: “On a scale of 0 to 10, how bad is your pain?” It is the medical version of “How’s the weather?” Simple, fast, and easy to squeeze into a busy visit. But for many patients, that number feels weirdly inadequate. A person can say “4” and still be unable to sleep, work, focus, or tie their shoes without gritting their teeth like a cartoon character trying to open a pickle jar. Another person can say “8” and still walk into the clinic, crack a joke, and insist they are “fine-ish.”
That is the problem. Pain is not just intensity. It is disruption. It is what pain does to your day, your movement, your mood, your relationships, your sleep, and your confidence. A one-number score may be convenient, but convenience is not the same as clarity. If the goal of pain care is to help people live better, then a better pain measure should track more than raw intensity alone.
So yes, it is time to replace the 0 to 10 pain intensity scale with something smarter. Not because intensity never matters, but because intensity by itself is too small a lens for a very big human experience.
Why the 0 to 10 pain scale feels broken
The numeric pain scale became popular because it is quick. It gives clinicians a standard prompt, helps document symptoms, and can be useful for rapid check-ins. In urgent settings, that speed matters. If someone just had surgery, broke a bone, or is recovering from a procedure, a fast question about pain severity can help guide immediate care.
But when that same scale becomes the main event, things start to wobble. Pain is subjective, personal, and shaped by context. A “6” for one person may feel like a “3” to someone else. Some people underrate pain because they do not want to sound dramatic. Others rate it high because the pain is frightening, exhausting, or constant. Neither person is wrong. They are just trying to squeeze a complicated reality into one lonely digit.
That single score also misses the question that often matters most: What is the pain stopping you from doing? If pain has gone from a 7 to a 5 but the patient still cannot walk the dog, lift a child, drive to work, or sleep through the night, has care meaningfully improved? Maybe a little. Maybe not enough. On the flip side, if pain stays at a 5 but the patient can now cook dinner, return to physical therapy, and stop canceling plans, that sounds like real progress.
In other words, the old scale is not exactly useless. It is just underqualified for the job.
One number cannot capture a whole pain story
Pain is more than sensation. It has physical, emotional, and social layers. It can flare with movement, worsen with stress, and feel dramatically different depending on whether someone is trying to rest, work, climb stairs, or sit through a meeting that should have been an email. A pain score alone does not tell you whether the pain is burning, stabbing, throbbing, constant, or unpredictable. It does not tell you whether the person is sleeping two hours a night or avoiding activity because they are afraid movement will make things worse.
That missing context matters. When pain assessment is too narrow, treatment decisions can become too narrow too. Care can drift toward chasing a lower number instead of chasing a better life.
What a better pain measure should actually include
If the 0 to 10 scale is too flimsy, what should replace it? A better measure should still include intensity, but it should place that number inside a fuller picture. Think of it as a small dashboard instead of a single blinking light.
1. Pain intensity
Yes, intensity still matters. A quick sense of severity can help spot changes, compare trends over time, and guide treatment. But intensity should be the opening question, not the entire interview.
2. Pain interference
This is the missing superhero in many pain conversations. Pain interference asks how much pain disrupts everyday life. Does it interfere with walking, getting dressed, working, concentrating, socializing, sleeping, or enjoying anything that used to feel normal? This is often more clinically useful than the intensity number alone because it shows whether pain is shrinking a person’s world.
3. Functional ability
Function is where pain care becomes real. Can the patient get out of bed more easily? Bend without panicking? Sit through a work shift? Carry groceries? Take a deep breath after surgery? A better pain measure should track what matters in daily life, not just what fits neatly on a chart.
4. Mood and stress
Pain and emotion are frequent roommates. Anxiety can amplify pain. Depression can make coping harder. Stress can crank the entire system into overdrive. If a measure ignores mood, it ignores one of the major forces shaping how pain is experienced and managed.
5. Sleep
Sleep and pain have a messy, mutually annoying relationship. Pain disrupts sleep, poor sleep increases distress, and the next day everything hurts more. A better measure should ask whether pain is waking the patient up, delaying sleep, or wrecking restorative rest.
6. Personal goals
This is the part medicine sometimes forgets and patients almost never do. Many people are not looking for a magical “zero pain” life. They want to garden again, sit through a soccer game, work a full shift, return to the gym, or make it through a family dinner without mentally planning an escape route. A better measure should include goals that are meaningful to the person, not just tidy for the chart.
The better alternative: measure pain, interference, and function together
If healthcare wants a practical replacement for the classic pain number, the smartest move is not to invent a dramatic new mystery scale with futuristic vibes. It is to use a brief, multidimensional measure that combines pain intensity with interference and function.
One strong model is a three-part check-in:
- How much pain are you having?
- How much is it interfering with your enjoyment of life?
- How much is it interfering with your general activity?
That simple structure is far more revealing than intensity alone. It keeps the speed of a short screening tool but adds the context clinicians actually need. If the pain number is high but interference is low, the plan may look different than if the pain number is moderate but the patient can no longer function at home or work.
For longer or more detailed visits, broader tools can go even further by looking at physical function, mood, sleep, daily activities, and pain behavior. The point is not to drown patients in paperwork. The point is to stop pretending a single number can carry the whole burden.
A smarter question changes the whole conversation
Imagine two patients both report a pain level of 6.
Patient A: “It’s a 6, but I’m sleeping okay, I can still work, and it eases when I move around.”
Patient B: “It’s a 6, but I haven’t slept through the night in a week, I’m skipping meals because cooking hurts, and I’m scared to bend over.”
Same number. Completely different clinical reality.
This is why better pain measurement matters. It helps separate pain that is uncomfortable from pain that is disabling, exhausting, destabilizing, or function-crushing. That leads to more tailored care, better follow-up, and fewer treatment decisions driven by guesswork.
Why this matters for patients, clinicians, and treatment decisions
Replacing the 0 to 10 pain scale is not just a paperwork upgrade. It changes how pain is treated. When clinicians focus only on lowering intensity, they may end up chasing the score instead of helping the person. That can encourage unrealistic expectations, especially in long-term pain conditions where the goal is often improved function, better coping, and safer, steadier daily living rather than total pain elimination.
A more complete measure also supports better conversations about treatment risk and benefit. If a medication lowers pain a bit but leaves the patient groggy, constipated, foggy, or no more functional than before, that is important. If physical therapy, pacing strategies, behavioral treatment, exercise, or a nonopioid option improves mobility and confidence even without producing a dramatic drop in the pain number, that matters too.
In other words, better measurement helps define better success. Success is not always “pain went from 8 to 2.” Sometimes success is “pain is still there, but now I can live with less fear, more movement, and fewer limitations.”
How clinics can replace the old scale without making visits longer
The good news is that this shift does not require turning every appointment into a 90-minute documentary. Clinics can adopt a layered approach.
Start with a short screening
Ask about pain intensity, pain interference with enjoyment of life, and pain interference with general activity. That alone is a major upgrade.
Add function-based follow-up questions
Ask one or two specific questions tied to daily life:
- What has pain made harder this week?
- What is one activity you want to do more comfortably?
- Are you sleeping, walking, working, or moving better than last visit?
Track trends, not just snapshots
Pain changes. A patient may feel worse in the morning, better after movement, and terrible after sitting too long. Trend data over time is more useful than one random number taken at 2:17 p.m. under fluorescent lights.
Make the goals personal
“Increase function” sounds nice in a policy document, but patients need something less robotic. Better goals sound like this: walk to the mailbox without stopping, sit through a school event, return to part-time work, sleep five nights a week without being woken by pain, or cook dinner without leaning on the counter like it is a life raft.
What patients can say instead of “It’s a 7”
Patients do not need a medical degree to help improve pain assessment. They just need permission to say more than a number.
Here are examples of better pain descriptions:
- “The pain is about a 5, but it spikes to an 8 when I climb stairs.”
- “It is not the intensity that bothers me most. It is that I can’t sleep.”
- “The pain is moderate, but it wipes out my focus by noon.”
- “I can tolerate the discomfort, but I’m avoiding movement because I’m afraid of making it worse.”
- “I’m okay at rest, but pain with activity is what’s limiting me.”
Those kinds of statements give clinicians something the old scale often cannot: a useful map.
Experiences from real-world pain conversations
Anyone who has lived with ongoing pain, cared for someone in pain, or worked in a setting where pain is discussed every day knows the 0 to 10 scale can produce some oddly theatrical moments. One patient says “10” while scrolling calmly through their phone. Another says “3” with tears in their eyes because they are embarrassed to complain. A stoic older adult shrugs and says, “Oh, it’s nothing,” then casually mentions they have not slept in three nights. A postoperative patient says “6,” but what they really mean is, “I can’t cough, I can’t laugh, and I am now negotiating peace terms with my own abdomen.”
These experiences are not proof that people are exaggerating or minimizing on purpose. They are proof that pain is deeply personal and wildly context-dependent. People rate pain through personality, culture, fear, past experience, expectations, and the situation they are in at that moment. Someone who has lived with chronic back pain for ten years may rate a flare very differently from someone experiencing intense pain for the first time. A parent trying to stay composed in front of a child may downplay pain. A person who has felt dismissed before may crank the number upward because they worry a “5” will be treated like a yawn.
Clinicians see this too. Many know that the most useful part of the pain discussion often begins right after the number. That is when patients explain that the pain is not constant, that it is worse with movement, that the real issue is not severity but sleep, or that the worst part is losing independence. Sometimes the number is almost an icebreaker, not the answer. The answer is in the follow-up: “What can’t you do because of it?” “What has changed since last time?” “What matters most to you right now?”
Caregivers often notice what the scale misses even faster. They see the skipped walks, the cautious way someone lowers into a chair, the abandoned hobbies, the shorter temper caused by exhaustion, and the quiet grief of no longer trusting one’s own body. None of that fits neatly inside a single digit. But all of it belongs in the assessment.
That is why people often feel relief when a clinician asks a more human question. Not just “How bad is it?” but “How is it affecting your life?” That question gives patients room to be honest. It turns the conversation from a performance into a partnership. And in many cases, that is the moment pain assessment finally starts to sound less like a pop quiz and more like actual care.
Conclusion
The 0 to 10 pain intensity scale had a good run. It is fast, familiar, and easy to document. But pain care has outgrown the idea that one number should lead the entire conversation. A better measure of pain should combine intensity with interference, function, sleep, mood, and patient-centered goals. It should ask not only how much pain hurts, but how much it steals.
If healthcare wants pain treatment to be safer, smarter, and more personal, the measurement has to improve first. Because when pain assessment gets better, decision-making gets better. And when decision-making gets better, patients have a better chance of getting something more meaningful than a lower score: a bigger life.