7 minutes ago 0
Jack Doherty went from filming flip tricks as a teenager to becoming one of the most talked-about...
Your Guide to Money & Cash Flow
 Jack Doherty Was Just A Kid With A Camera, And Now His Net Worth Is Raising Eyebrows
Jack Doherty Was Just A Kid With A Camera, And Now His Net Worth Is Raising Eyebrows  “Was Immediately T-Boned”: 29 People Recall Moments When Karma Came For People Instantly
“Was Immediately T-Boned”: 29 People Recall Moments When Karma Came For People Instantly 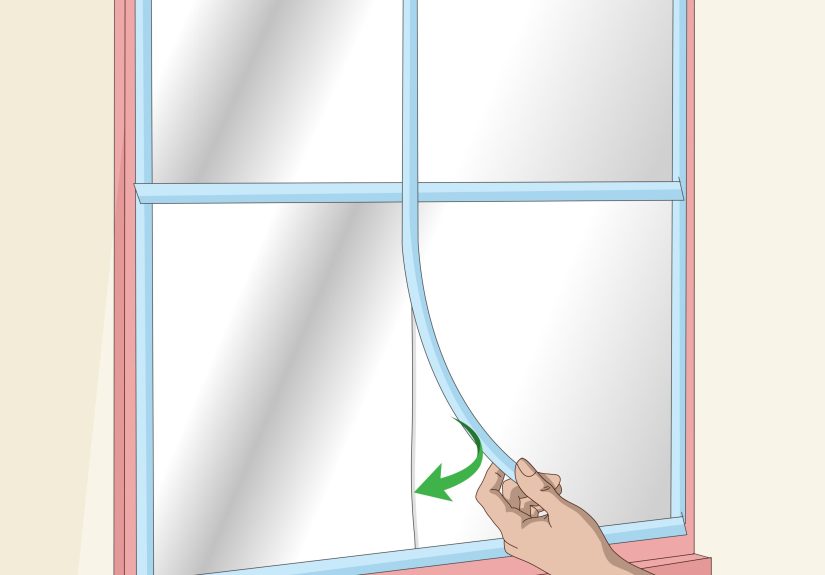 How to Wrap Windows with Aluminum: 11 Steps
How to Wrap Windows with Aluminum: 11 Steps  Living with a Behcet’s disease diagnosis
Living with a Behcet’s disease diagnosis  Dear SaaStr: How Do You Evaluate Startups for Seed Investments?
Dear SaaStr: How Do You Evaluate Startups for Seed Investments?