Table of Contents >> Show >> Hide
- What is the TMJ, and what are TMJ disorders?
- Common causes and risk factors
- Signs and symptoms you shouldn’t ignore
- How TMJ disorders are diagnosed
- Treatment options: from simple to more involved
- When to see a doctor or dentist about jaw pain
- Everyday habits to protect your jaw
- Real-life experiences with TMJ disorders: what living with jaw pain feels like
- Putting it all together
If you’ve ever yawned, heard a loud click in your jaw, and thought, “Well that can’t be good,” you’re not alone. Temporomandibular joint (TMJ) disorders are a common cause of jaw pain, headaches, and that charming habit of massaging your face in public. The good news: while TMJ disorders can be frustrating and painful, many people find relief with simple, conservative treatments and a few lifestyle tweaks.
In this guide, we’ll break down what TMJ disorders are, what causes them, the most common symptoms, and practical ways to manage and relieve TMJ pain. We’ll also walk through real-life experiences so you can see what living with TMJ issues is really likeand why there’s plenty of reason to be hopeful.
What is the TMJ, and what are TMJ disorders?
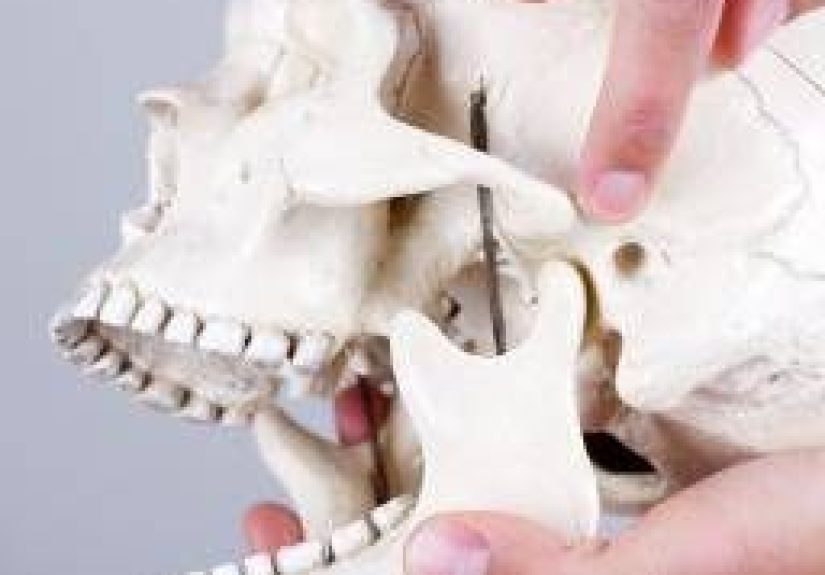
The temporomandibular joints are the small but mighty hinges that connect your lower jaw (mandible) to the temporal bones of your skull, just in front of each ear. A smooth cartilage disc helps the joint glide so you can talk, chew, yawn, sing in the car, and complain about your internet speed without pain or grinding.
“TMJ” technically refers to the joint itself, while “TMD” (temporomandibular disorders) refers to the group of conditions that cause pain or dysfunction in the joint and the muscles that control jaw movement. Experts describe more than 30 different TMD conditions, but most fall into three main categories:
- Jaw muscle disorders (myofascial pain) – tight, painful muscles in the jaw, face, neck, or shoulders.
- Joint disorders – problems with the cartilage disc or joint surfaces, such as displacement or degeneration.
- Joint disease or injury – arthritis, trauma, or other structural problems affecting the joint.
TMJ disorders are fairly common. They’re seen more often in adults, particularly between the ages of 20 and 40, and may occur more frequently in women than in men.
Common causes and risk factors
One of the trickiest things about TMJ disorders is that there usually isn’t a single, simple cause. Instead, several factors often pile up over timelike stress, posture, and habitsuntil the jaw finally starts to complain.
1. Jaw strain and overuse
Many TMJ problems start with overworked jaw muscles or joints. That can happen when you:
- Clench or grind your teeth (bruxism), especially at night.
- Chew gum or ice constantly.
- Take very large bites or chew tough, sticky foods often.
- Hold the jaw in a tense position during stress.
Over time, this constant strain can irritate the muscles and the joint, leading to pain, stiffness, and clicking or popping noises.
2. Structural or joint problems
Sometimes the issue lies in the joint itself. For example:
- Disc displacement – the cartilage disc that cushions the joint can slip out of place, causing clicking, popping, or locking.
- Arthritis – osteoarthritis or inflammatory arthritis can damage the TMJ, just as they affect other joints.
- Jaw injury – a blow to the face, whiplash, or a broken jaw can damage the joint and surrounding tissues.
- Jaw shape and bite issues – some people have smaller lower jaws or certain bite patterns that may increase stress on the TMJ.
3. Medical conditions and other triggers
Other health issues and situations can contribute to TMJ problems, including:
- Autoimmune conditions that affect joints.
- Infections in or around the joint (less common).
- Long dental procedures that require holding the mouth open for a long time.
- Stress and anxiety that lead to clenching, grinding, or tense jaw muscles.
Signs and symptoms you shouldn’t ignore
TMJ disorders don’t look the same in everyone. Some people mainly notice jaw pain; others notice headaches or ear symptoms first. Common signs and symptoms include:
- Dull, aching pain in the jaw, face, or around the ears.
- Jaw stiffness or a feeling that the jaw is “tired.”
- Clicking, popping, or grinding sounds when opening or closing the mouth.
- Difficulty or pain when chewing, talking, or yawning.
- Locking of the jaw (getting stuck open or closed, even briefly).
- Headaches or migraines, especially around the temples.
- Ear symptomsfullness, ringing (tinnitus), or earaches without infection.
- Neck or shoulder pain that seems connected to jaw tension.
One important note: not every jaw click means you have a TMJ disorder. If your jaw makes noise but you don’t have pain or difficulty moving it, many experts consider that normal and not necessarily a condition that needs treatment.
How TMJ disorders are diagnosed
There’s no single “TMJ test,” so diagnosis is mostly about putting the pieces together: your symptoms, your history, and a careful exam.
Medical and dental history
Your dentist, primary care provider, or a specialist will usually start by asking detailed questions, such as:
- When did the pain or clicking start?
- Does the pain come and go, or is it constant?
- Does anything make it better or worse (chewing, yawning, stress)?
- Do you grind or clench your teeth, or has anyone told you that you do?
- Have you had any injuries to your face or jaw?
Physical exam
During the exam, your provider may:
- Feel the joints and jaw muscles while you open and close your mouth.
- Listen for clicks, pops, or grinding noises.
- Measure how wide you can open your mouth.
- Check your bite and look for signs of grinding on your teeth.
- Assess your neck, head, and posture, since they often play a role.
Imaging and other tests
Most people with TMJ disorders don’t need extensive imaging right away. But if your symptoms are severe, long-lasting, or unusual, your provider may order:
- X-rays to look at the bones of the jaw.
- CT scans for detailed images of the joint structure.
- MRI to evaluate the cartilage disc and soft tissues.
Because TMD can overlap with other pain conditions (like headaches, ear disorders, or neck problems), you may also see other specialists, such as a physical therapist, ENT specialist, or pain specialist, as part of a team-based approach.
Treatment options: from simple to more involved
Here’s some encouraging news: many TMJ disorders improve over timeoften with conservative, reversible treatments. Major organizations recommend avoiding aggressive, permanent procedures unless all simpler options have been tried and carefully evaluated.
Self-care and home remedies for TMJ pain
If your provider suspects a TMJ disorder, they’ll almost always start with home-based and lifestyle strategies, such as:
- Soft diet – temporarily choose softer foods (soups, yogurt, eggs, cooked vegetables) and cut food into smaller pieces. Avoid very chewy or sticky foods like bagels, tough steak, and gum.
- Jaw rest – avoid wide yawning, singing loudly, biting your nails, or holding your phone between your shoulder and jaw.
- Heat and cold – warm, moist heat can relax tight muscles; cool packs can help with sharp pain and inflammation.
- Over-the-counter pain relievers – nonsteroidal anti-inflammatory drugs (NSAIDs), like ibuprofen, may help short term when used as directed.
- Gentle stretching and massage – a physical therapist or trained provider can teach you specific jaw stretches and muscle massage techniques.
- Stress management – relaxation exercises, deep breathing, or mindfulness can reduce tension that leads to clenching.
- Posture check – keeping your head stacked over your shoulders, especially at a computer, can reduce strain on jaw and neck muscles.
These steps may sound simple, but for many people they make a noticeable difference within a few weeks.
Professional treatments that may help
If home care isn’t enough, your provider may recommend additional options, such as:
- Splints or night guards – custom-made oral appliances worn over the teeth can reduce clenching forces, protect your teeth, and sometimes relieve joint pressure.
- Physical therapy – targeted exercises, manual therapy, and posture training can improve jaw movement and reduce pain.
- Medications – short-term use of prescription muscle relaxants, certain antidepressants (for chronic pain), or other medications may be considered as part of a broader plan.
- Counseling or behavioral therapy – cognitive behavioral therapy (CBT), biofeedback, and other techniques can help you recognize and change habits like clenching, and manage chronic pain more effectively.
- Injections or minimally invasive procedures – in selected cases, providers may consider injections into the joint or procedures such as arthrocentesis (flushing the joint). These are usually reserved for specific, persistent problems after conservative care.
Treatments to approach with caution
Because the science around TMJ disorders is still evolving, experts strongly recommend avoiding irreversible treatments unless there’s a clear medical need and strong supporting evidence. These include:
- Permanent bite changes (large tooth reshaping or extensive crowns solely “for TMJ”).
- Orthodontic treatment that is done only to “fix TMJ” without clear evidence it will help.
- Major jaw surgery or joint replacement unless you have a severe, well-documented joint disease and conservative options have been exhausted.
Before agreeing to any permanent or invasive treatment, it’s reasonable to ask for a second opinionideally from a provider familiar with current TMJ research.
When to see a doctor or dentist about jaw pain
Not every brief jaw twinge needs an urgent visit. But you should schedule an appointment with your dentist, primary care provider, or a TMJ specialist if you:
- Have jaw pain or stiffness that lasts more than a couple of weeks.
- Notice your jaw frequently clicks, pops, or feels unstable.
- Have difficulty chewing because of pain or limited opening.
- Experience jaw locking (even briefly).
- Have headaches, ear pain, or facial pain that seem linked to jaw movement.
- Can’t open your mouth wide enough to eat comfortably.
Seek urgent or emergency care if jaw pain comes on suddenly after a facial injury, if your jaw becomes stuck and you can’t close your mouth at all, or if jaw pain is accompanied by chest pain, shortness of breath, or other signs that might suggest a heart problem.
Everyday habits to protect your jaw
Think of your TMJ as a small hinge that appreciates good manners. These habits can reduce strain and help prevent flare-ups:
- Keep a “relaxed jaw” posture – lips together, teeth slightly apart, tongue resting gently on the roof of the mouth.
- Limit gum chewing – save it for special occasions, not an all-day habit.
- Avoid biting non-food items – pens, ice cubes, fingernails, and bottle caps are all off the menu.
- Cut food into smaller pieces – especially crusty bread, big sandwiches, or thick burgers.
- Watch your screen posture – adjust your chair, screen, and keyboard so your head isn’t jutting forward.
- Manage stress – incorporate short relaxation breaks, gentle stretching, or calming routines into your day.
- Protect your sleep – good sleep hygiene (regular schedule, comfortable pillow, limiting screens before bed) may help reduce nighttime clenching.
Real-life experiences with TMJ disorders: what living with jaw pain feels like
Reading about causes and treatments is helpful, but TMJ disorders are ultimately a day-to-day experience. Everyone’s journey is slightly different, yet many people share common themes: frustration, trial-and-error, and eventually, a workable routine that keeps symptoms in check.
“I thought it was just stress”
Alex, a 32-year-old graphic designer, first noticed jaw pain during a particularly busy month at work. The deadlines were tight, meals were rushed, and late-night coffee had turned into an everyday event. The first sign wasn’t painit was a loud click whenever Alex yawned. A few weeks later, chewing a bagel felt like a workout.
At first, Alex ignored it and chalked it up to stress. But then came the morning headaches and a stiff neck. A visit to the dentist revealed noticeable wear on the teeth, suggesting nighttime clenching. The dentist recommended a night guard and a soft diet for a few weeks, plus simple jaw stretches and shorter breaks away from the computer.
The change didn’t happen overnight. But over two to three months, the combination of better posture, a night guard, and some honest conversations about stress at work led to noticeable improvement. The jaw still clicks sometimes, but the pain is rareand now it’s a gentle reminder to schedule a break instead of another all-nighter.
“It wasn’t just my jawit affected everything”
Maria, a 45-year-old teacher, developed TMJ pain after a minor car accident. At first, she assumed it was just whiplash. But as weeks went by, chewing became uncomfortable, her jaw felt stiff, and she started waking up with earache-like pain that antibiotics never fixed.
Maria eventually met with a multidisciplinary team that included a physical therapist, a dentist familiar with TMJ disorders, and a pain specialist. Together, they focused on gentle jaw mobilization, neck and upper-back exercises, stress management, and a short course of medication to calm down irritated muscles.
The emotional side surprised her. Constant low-level pain made her more irritable and tired, and she worried about long-term damage. A therapist helped her untangle fears about “ruining” her jaw and gave her practical tools for pacing activities and relaxing her muscles when she felt tension creeping in.
Over time, her pain dropped from a constant 7 out of 10 to a 1 or 2 on most dayssometimes zero. She still avoids very chewy foods and knows that stressful weeks can cause a flare-up. But now she sees those flares as signals to slow down, not signs that things are permanently getting worse.
“Small daily habits made the biggest difference”
Jordan, a college student, discovered just how much small habits can affect the jaw. Between studying, gaming, and scrolling on a laptop in bed, their posture was almost always “chin forward, shoulders hunched.” They also chewed gum for hours and often caught themselves clenching during exams.
After TMJ symptoms kicked injaw clicking, tension headaches, and a dull ache near the earsJordan’s dentist suggested an experiment: two weeks of no gum, a “lips together, teeth apart” jaw posture rule, and two 5-minute posture breaks every hour while studying.
The first week felt annoying and unnatural. By the third week, though, the jaw felt less tight, headaches decreased, and Jordan realized just how often stress landed in their jaw muscles. Continuing those small habits, along with occasional physical therapy, became the cornerstone of long-term relief.
These experiences share a few consistent threads:
- Relief usually comes from a combination of strategies, not one magic fix.
- Conservative, reversible treatments often work well over time.
- Stress, posture, and daily habits matter just as much as what’s happening inside the joint.
- Feeling informed and supported makes the journey much less scary.
Putting it all together
TMJ disorders can be painful, annoying, and occasionally loud (that click has a flair for drama). But they’re also manageable in many cases, especially when you address them early and take a “less is often more” approach to treatment.
If you’re dealing with jaw pain, stiffness, or unexplained headaches, start by talking with a dentist or healthcare provider who’s familiar with TMJ disorders. Focus first on simple steps: a softer diet for a while, good posture, stress management, gentle jaw exercises, and possibly a night guard if you clench or grind.
Most importantly, remember that you don’t have to figure it out alone. With the right information, a supportive care team, and a bit of patience, many people find steady, long-lasting reliefand get back to eating, laughing, and yawning without worrying what their jaw will do next.