Table of Contents >> Show >> Hide
- First, a 10-second anatomy refresher
- When it’s an emergency right now
- Risk factors: Who is most likely to swallow or inhale something?
- Symptoms: How you can tell whether it’s swallowed vs inhaled
- The “high-risk object” hall of fame
- How doctors diagnose a swallowed or inhaled foreign object
- Treatment: What happens next depends on what it is and where it is
- What not to do at home
- Prevention: boring advice that saves the day
- Conclusion
- Experiences: What these situations often look like in real life (and what people learn)
Your body is excellent at swallowing food and breathing air. It is less thrilled when you mix up the
assignment and send a coin, a chicken bone, or a button battery down the wrong “tube.” When something gets
swallowed into the digestive tract (foreign body ingestion) or inhaled into the airway (foreign body aspiration),
the best outcome is a quick fix and a great story later. The worst outcome is an emergency that needs fast,
expert care.
This guide breaks down the biggest risk factors, what symptoms to watch for, how doctors figure out where the
object went, and what treatment typically looks likeespecially for high-risk items like button batteries and
magnets. (Spoiler: those two are the overachievers of causing serious harm.)
First, a 10-second anatomy refresher
From the mouth, there are two main paths:
- Esophagus → stomach → intestines (swallowed object)
- Trachea/windpipe → bronchi → lungs (inhaled/aspirated object)
Sometimes a swallowed object gets stuck in the throat or esophagus. Sometimes it reaches the stomach and passes
on its own. And sometimes an “I swallowed it” situation is actually “I inhaled it,” especially in kids who choke,
cough, and then suddenly seem “fine”… until the wheezing or pneumonia shows up later.
When it’s an emergency right now
Call 911 (or your local emergency number) immediately if any of these are happening:
- Choking with inability to breathe, speak, or cough effectively
- Blue/gray lips or face, severe breathing trouble, or sudden collapse
- Drooling and inability to swallow saliva
- Severe chest/neck pain with trouble swallowing
- Suspected button battery ingestion (especially if it could be lodged in the esophagus)
- Suspected ingestion of multiple magnets or a magnet plus metal object
Button batteries can cause severe caustic injury in as little as two hours if stuck in the
esophagus, so “wait and see” is not the vibe here.
Risk factors: Who is most likely to swallow or inhale something?
1) Babies and toddlers (the “everything is a snack” phase)
Children under about age 4 are at higher risk because they explore with their mouths, move fast, and do not come
with factory-installed judgment. Coins, small toy parts, jewelry, and batteries are common culprits.
Aspiration risk spikes when kids are eating while laughing, running, climbing, or doing their best impression of
a tiny unicycle performer. Round and slippery foods like grapes and hot dog pieces, plus peanuts and popcorn, are
classic choking/aspiration hazards.
2) Older adults and anyone with swallowing problems
Adults can accidentally swallow foreign objects toooften fish bones, chicken bones, or dental appliances.
Risk rises with:
- Dental issues or dentures (reduced sensation while chewing)
- Dysphagia (swallowing difficulty) from stroke, Parkinson’s, dementia, or neuromuscular disease
- Esophageal narrowing (strictures), inflammation, or conditions that make food stick
- Intoxication/sedation (slower reflexes, poorer coordination)
Aspiration (food/liquid going into the airway) is also more likely when swallowing coordination is impaired, and
it can lead to airway blockage or infection like aspiration pneumonia.
3) Situational and behavioral risk factors
- Eating too fast (hello, steak “food bolus” impaction)
- Talking/laughing while chewing
- Small batteries and high-powered magnets in the home (toys, remotes, key fobs, greeting cards)
- Children with access to older siblings’ toys (tiny parts migrate like glitter)
Symptoms: How you can tell whether it’s swallowed vs inhaled
Common symptoms of a swallowed foreign object
- Difficulty swallowing, drooling, gagging
- Chest/throat/neck pain
- Vomiting or refusing food (especially in children)
- Abdominal pain
- Sometimes: very mild symptoms at first, then worsening inflammation/infection later
Mild early symptoms don’t always mean “all clear.” Some objects are forgotten until pain, fever, vomiting, or
other symptoms develop later.
Common symptoms of an inhaled/aspirated foreign object
- Sudden coughing or choking episode
- Wheezing, noisy breathing, or stridor
- Difficulty speaking or breathing
- Persistent cough that “won’t quit”
- Recurrent pneumonia or one-sided wheeze (especially if the event wasn’t witnessed)
An inhaled object can initially cause dramatic chokingor surprisingly subtle symptomsbefore progressing to
inflammation or infection.
The “high-risk object” hall of fame
Button batteries: tiny, shiny, and medically terrifying
Button battery ingestion is treated as an emergency because a battery lodged in the esophagus can generate a
strong alkaline injury that burns tissue quickly, potentially leading to perforation or even life-threatening
complications.
What to do if you suspect a button battery was swallowed:
- Go to the ER immediately (do not wait for symptoms).
- Do not induce vomiting.
- Call Poison Control (in the U.S., Poison Help is commonly reached through national poison resources).
-
If the child is 12 months or older, some poison-control guidance supports giving honey while
heading to the ER in specific situationsbut never delay getting emergency care.
Magnets: the “buddy system” that can destroy intestines
A single small magnet may pass, but two or more magnets (or a magnet plus a metal object) can
attract each other across loops of intestine. That can pinch tissue, cut off blood flow, and cause perforations
or infectionsometimes requiring surgery.
Sharp or pointed objects
Fish bones, toothpicks, needles, pins, and broken plastic can scratch, puncture, or get stuck. Sharp objects in
the esophagusor signs of injurytypically call for urgent medical evaluation and often removal.
Large objects and food impaction
Long or bulky items can lodge in the esophagus or have trouble navigating the GI tract. Food impaction (often
meat) can feel like something is stuck behind the breastbone, with drooling or inability to swallow liquids. That
can require urgent endoscopic treatment.
How doctors diagnose a swallowed or inhaled foreign object
Step 1: History and “object detective work”
Clinicians want to know: What was involved (coin vs battery vs magnet), when
it happened, and what symptoms occurred right away (choking, coughing, drooling, pain). If the object is unknown,
doctors often assume the “most dangerous plausible option” until proven otherwiseespecially for coin-shaped
objects that could actually be button batteries.
Step 2: Imaging
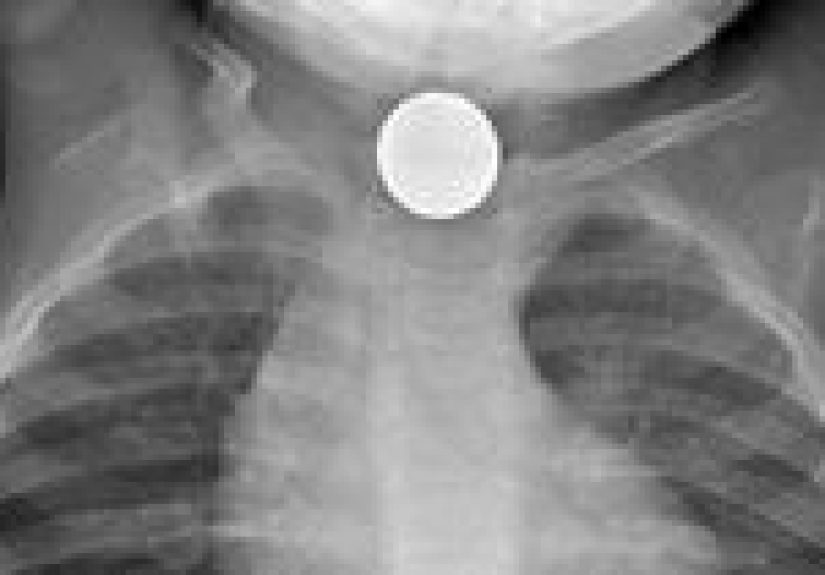
X-rays are commonly used to locate metal objects and see whether something is in the airway, esophagus, stomach,
or intestines. Many pediatric protocols recommend a series of views (neck/chest/abdomen) when the location is
unclear, and immediate imaging when a high-risk object is suspected.
If the object is radiolucent (not easily seen), or if aspiration is suspected but X-rays are inconclusive, CT or
other imaging may be consideredespecially when symptoms persist.
Step 3: Endoscopy or bronchoscopy (the “go get it” step)
If an object is stuck in the esophagus, dangerous, or causing symptoms, doctors may use:
- Endoscopy to remove objects from the esophagus/stomach/upper intestine
- Bronchoscopy to remove objects from the airway (often the standard for aspiration cases)
In children with foreign body aspiration, bronchoscopy is commonly the standard removal method.
Treatment: What happens next depends on what it is and where it is
1) If it’s in the airway: stabilize first, then remove
A complete airway blockage is an emergency requiring immediate first aid (age-appropriate choking response) and
emergency services. After stabilization, aspiration is usually treated by removing the object, often with
bronchoscopy.
If the object has been there a while, doctors may also treat complications like airway swelling, atelectasis
(collapsed lung segment), or infection. Aspiration pneumonia, when present, is treated medically (often with
antibiotics) based on clinical findings.
2) If it’s stuck in the esophagus: it often needs prompt removal
Objects lodged in the esophagus are more likely to cause pain, drooling, and obstructionand they’re less likely
to pass on their own. Button batteries in the esophagus are removed emergently. Many other esophageal foreign
bodies (especially symptomatic ones) are removed urgently using endoscopy.
3) If it reached the stomach: sometimes observation is appropriate
Many small, smooth objects that have made it into the stomach will pass through the intestines without incident.
In those cases, clinicians may recommend observation with clear return precautions. (Translation: “If pain,
vomiting, fever, blood, or new symptoms show up, come backimmediately.”)
That said, location isn’t the only factorobject type matters. Batteries, magnets, sharp objects,
and large items may still need removal even if they’ve reached the stomach, depending on size, age, symptoms, and
whether the object is progressing on follow-up imaging.
4) Surgery: uncommon, but sometimes necessary
Surgery is typically reserved for complications (perforation, obstruction, abscess) or for objects that cannot be
safely removed endoscopicallysuch as severe injuries from multiple magnets. The good news is that surgery is the
exception rather than the rule, but the “danger objects” list (batteries, magnets, sharp items) is exactly why
prompt evaluation matters.
What not to do at home
- Do not induce vomiting (especially dangerous for batteries and sharp objects).
- Do not “push it down” with food or bread if someone is struggling to swallow or drooling.
- Do not assume “no symptoms” means “no problem” after possible aspiration or battery ingestion.
-
Do not delay care for suspected button batteries or multiple magnetstime is a major factor in
preventing severe injury.
Prevention: boring advice that saves the day
Childproofing that actually works
- Keep button batteries locked up and ensure battery compartments are secured.
- Keep high-powered magnet sets away from children (and treat missing magnets as a “search party” situation).
- Follow age labels on toyssmall parts and toddlers are a classic bad pairing.
- Cut round foods (grapes, hot dogs) into safer shapes; supervise meals and snacks.
Pediatric safety guidance consistently emphasizes that button batteries are an emergency if swallowed and should
be kept out of reach and secured in devices.
For adults and caregivers
- Address swallowing difficulties early (speech/swallow evaluation can be life-changing).
- Chew slowly, especially if you wear dentures or have known esophageal issues.
- Seek care promptly if food repeatedly “gets stuck” (that may signal an underlying condition).
Conclusion
Swallowing (or inhaling) a foreign object ranges from “it’ll pass” to “go now.” The difference comes down to the
object, the location, and the symptoms. Smooth items in the stomach may be observed, but anything that causes
breathing trouble, drooling, inability to swallow, or severe pain deserves urgent medical attention. And if the
object might be a button battery or multiple magnets, treat it as an emergency
even if the person looks okaybecause the damage can start quickly and quietly.
Experiences: What these situations often look like in real life (and what people learn)
Experience #1: “I’m pretty sure it was a coin.”
A parent hears the clink, sees the guilty toddler face, and finds an open remote control nearby. The child seems
mostly finemaybe a little drooly, maybe a little fussy. In the ER, the X-ray reveals the coin-shaped object is a
button battery. The takeaway that hits hardest: lack of dramatic symptoms doesn’t equal lack of danger.
Families often say the most useful phrase they learned is, “Assume battery until proven otherwise,” especially
when the object is shiny and coin-sized.
Experience #2: The “silent aspiration” surprise.
A child chokes while eating peanuts, coughs hard, then bounces back like nothing happened. Everyone exhales. A
week later, there’s a persistent cough and a wheeze that doesn’t respond the way asthma usually does. In these
stories, caregivers often wish they had trusted the original choking episode more than the quick recovery. What
changes future behavior is simple: if there’s a clear choking event followed by ongoing cough, wheeze, or fever,
they ask specifically about foreign body aspirationbecause airway objects can hide out and cause trouble later.
Experience #3: “It’s just food stuck… right?”
Adults often describe food impaction as a sudden, uncomfortable “pressure” behind the breastbone, sometimes with
the inability to swallow even saliva. People try sips of water, more bites of food, or repeated swallowing.
Eventually they realize it’s not budgingand the drooling is a clue that it’s time for urgent evaluation. After
an endoscopic removal, many patients learn they have an underlying issue (like narrowing or inflammation) that
made the esophagus more likely to trap food. The lesson they share: the ER visit wasn’t just about removing the
stuck bite; it was about preventing repeat episodes and complications.
Experience #4: The magnet “I didn’t think it mattered” moment.
With magnets, the story is often delayed: vague belly pain, intermittent vomiting, and a caregiver who doesn’t
recall a clear ingestion event. Then imaging shows multiple magnets. Families who go through this frequently
become magnet-safety evangelists afterwardchecking toy sets, counting pieces, and treating “missing magnets” as a
real problem, not a minor mystery. The consistent insight: magnets are deceptive because they don’t just block
the gut; they can pinch it from the inside.
Experience #5: Recovery is a process, not a single event.
When injuries occurespecially from button batteriespeople are often surprised that treatment doesn’t always end
with removal. Follow-up can include repeat evaluations for scarring or narrowing, diet changes while tissues heal,
and careful monitoring for delayed complications. Families frequently say the most helpful thing they did was keep
a simple timeline: what was swallowed, when it happened, symptoms noticed, and what the hospital found. That
record helps clinicians make safer decisions and helps caregivers feel less powerless in a scary situation.
If there’s one common thread across these experiences, it’s this: people don’t regret getting evaluated “too
early.” They regret waiting when the object was high-risk, the symptoms were subtle, or the choking episode felt
like it “passed.” Your instincts plus prompt medical assessment is a strong team.





