Table of Contents >> Show >> Hide
- What “Skin Neoplasm” Actually Means (and Why It’s So Broad)
- The Four Behavior Buckets: A Practical Map
- Common Benign Skin Neoplasms (and Why They Still Get Checked)
- Malignant Skin Neoplasms: What They Are and What They Often Look Like
- “Uncertain Behavior” on a Pathology Report: What It Usually Means Next
- Skin Cancer Risk: What Actually Raises the Odds
- How Dermatologists Evaluate a Suspicious Skin Neoplasm
- ABCDE and Other Warning Signs You Can Use at Home
- Prevention and Risk Reduction That Actually Helps
- When to See a Dermatologist (Sooner Rather Than Later)
- Real-World Experiences (Common Stories People Share) 500+ Words
- Conclusion
The phrase “skin neoplasm” can sound like something that should come with dramatic music and a
slow zoom. In real life, it’s usually less “movie trailer” and more “medical shorthand.” A skin neoplasm simply
means an unusual growth made of skin (or skin-related) cells. That growth might be harmless,
might be cancer, or might land in the frustrating middle category: uncertain behavior.
This guide breaks down what those labels really mean, why “uncertain behavior” shows up on pathology reports,
what actually increases skin cancer risk, and how to decide when a spot deserves a quick photo
for monitoring versus a fast appointment with a dermatologist. (Spoiler: your skin is allowed to be weird. It’s
just not allowed to be weird quietly.)
What “Skin Neoplasm” Actually Means (and Why It’s So Broad)
In plain English, a neoplasm is a new growth of tissue caused by cells multiplying more than they
should. It’s a category label, not a verdict. Think of it like “vehicle”: it could be a bicycle, a sedan, a bus,
or a rocket ship. You need more details before you know how worried (or annoyed) you should be.
Clinicians and pathologists usually describe skin neoplasms by behavior:
benign (not cancer), malignant (cancer), precancerous (not
cancer yet, but has potential), and uncertain behavior (not enough evidence to confidently call it
benign or malignant based on what’s been sampled).
The Four Behavior Buckets: A Practical Map
1) Benign: The “Not Cancer” Club
Benign skin neoplasms are noncancerous growths. They don’t invade nearby tissue or spread to other
parts of the body. Many are common, especially with age and sun exposure. Some are removed because they itch, snag,
bleed, grow, or just look suspicious enough that nobody wants to guess.
Important nuance: “Benign” does not always mean “ignore forever.” It means the growth is not behaving like cancer.
But a benign growth can still be annoying, infected, irritated, or mistaken for something more serious.
2) Malignant: Skin Cancer (and Why Early Matters)
Malignant skin neoplasms are cancers. The most common types include:
basal cell carcinoma (BCC), squamous cell carcinoma (SCC), and
melanoma. BCC and SCC are far more common than melanoma, but melanoma tends to be more dangerous
if not caught early.
3) Precancerous: The “Not Yet, But Don’t Ignore Me” Category
Some lesions aren’t cancer but have the potential to become cancer over time. A classic example is
actinic keratosis, a rough, sun-damaged patch that can progress to SCC in some cases.
Another is squamous cell carcinoma in situ (confined to the top layer of skin), which is treated
to prevent invasion.
4) Uncertain Behavior: The “We Need More Clues” Label
A neoplasm of uncertain behavior of skin often means the lab can’t confidently predict how the
lesion will act based on the current sample. This can happen when:
- The biopsy was partial (the most worrisome area might not have been captured).
- The features are borderlinenot clearly benign, not clearly malignant.
- The lesion type is rare or doesn’t fit neatly into a standard box.
- Inflammation, scarring, or prior treatment makes interpretation harder.
You may also see pathology terms like “atypical melanocytic proliferation” or
“melanocytic tumor of uncertain malignant potential”. These phrases can sound ominous, but they
often reflect diagnostic caution: the pathologist is flagging that the lesion deserves a more complete removal,
closer review, or follow-upbecause certainty matters.
In billing and coding, “uncertain behavior” can also appear as an ICD-10-CM diagnosis code (for example,
D48.5 for neoplasm of uncertain behavior of skin). That code doesn’t automatically mean “you have
cancer.” It often means “the final behavior is not confirmed yet.”
Common Benign Skin Neoplasms (and Why They Still Get Checked)
Many benign growths are so common that dermatologists could probably identify them from space. Still, benign
lesions sometimes mimic skin cancer, and cancer can occasionally masquerade as something “normal.” Here are a few
frequent benign suspects:
Seborrheic Keratosis: The “Stuck-On” Classic
Seborrheic keratoses are common, noncancerous growths that often look waxy, scaly, or “pasted on.”
They can be tan, brown, or black and tend to increase with age. They’re usually harmless, but they can itch, get
irritated, or look alarming enough to warrant a quick lookespecially if one changes suddenly.
Dermatofibroma: The Small, Firm Bump That Won’t Quit
A dermatofibroma is typically a firm, small bump, often on the legs, that may develop after minor
skin trauma (like a bug bite). It’s usually benign. Some variants (like cellular dermatofibroma) may prompt a more
careful evaluation because they can resemble other conditions.
Skin Tags, Cherry Angiomas, Lipomas, and Cysts
Skin tags are soft little growths in friction areas (neck, underarms). Cherry angiomas
are bright red vascular spots. Lipomas are soft fatty lumps under the skin. Epidermoid cysts
(often called “sebaceous cysts,” though that term isn’t always accurate) are typically slow-growing bumps that can
inflame or rupture. None of these are automatically dangerousbut anything that rapidly grows, bleeds without a
clear reason, or changes in an unusual way deserves evaluation.
Malignant Skin Neoplasms: What They Are and What They Often Look Like
Basal Cell Carcinoma (BCC)
BCC is the most common skin cancer in the U.S. It often appears on sun-exposed areas and may look
like a pearly bump, a sore that doesn’t heal, or a shiny patch. BCC tends to grow slowly and is highly treatable,
but it can cause local damage if ignored.
Squamous Cell Carcinoma (SCC)
SCC often shows up as a scaly patch, a crusted growth, or a persistent sorecommonly on areas with
lots of sun exposure (face, ears, neck, hands). SCC can be more aggressive in some situations, especially in people
with weakened immune systems, so early treatment matters.
Melanoma
Melanoma starts in pigment-producing cells (melanocytes). It’s less common than BCC or SCC but
accounts for a larger share of skin cancer deaths. Melanoma can appear as a new dark spot, a changing mole, or an
unusual lesion that stands out from the rest.
“Uncertain Behavior” on a Pathology Report: What It Usually Means Next
If your report includes “uncertain behavior,” the next step is often about getting a clearer answernot living in
limbo. Common next moves include:
- Complete excision: removing the remaining lesion with a margin so the pathologist can examine the whole thing.
- Second pathology review: sometimes a dermatopathologist (a pathologist specializing in skin) is asked to review tricky cases.
- Close clinical follow-up: if the lesion is fully removed and features suggest very low risk, monitoring may be recommended.
Why the caution? Because tiny differences under the microscope can change management. A partial sample might show
atypical features, but the full lesion may reveal a reassuring patternor confirm a malignancy that needs more
treatment. In other words: uncertain behavior is often a signal to finish the investigation, not a
diagnosis of doom.
Skin Cancer Risk: What Actually Raises the Odds
Risk isn’t about one thing. It’s a pile-up of exposures, biology, and history. Key risk factors include:
Ultraviolet (UV) Exposure (Sun and Indoor Tanning)
UV radiation is a major driver of many skin cancers. Cumulative sun exposure matters, and indoor tanning devices
expose users to intense UV. “Base tans” don’t protect you; they’re evidence of skin damage. If your goal is “bronze,”
consider self-tanner. If your goal is “keep your cells from freelancing,” avoid tanning beds.
History of Sunburns (Especially Blistering Sunburns)
Past sunburnsparticularly severe onesare associated with higher skin cancer risk. This is one reason dermatologists
take a sunburn history seriously, even if the burns happened years ago.
Skin Type and Pigment
People with lighter skin that burns easily have higher rates of BCC, SCC, and melanoma. But skin cancer can occur in
any skin tone. In darker skin, cancers may show up in less sun-exposed areas (like palms, soles, or under nails),
and diagnosis can be delayed if people assume risk is “zero.” It isn’t.
Many Moles or Atypical (Dysplastic) Nevi
Having many moles can increase melanoma risk. Atypical moles (dysplastic nevi) are also linked to a
higher riskespecially if you have several of them. This doesn’t mean an atypical mole is melanoma, but it does mean
monitoring and professional exams become more important.
Age, Immune System, and Medical History
Skin cancer risk rises with age, partly due to cumulative UV exposure. People with weakened immune systems (for
example, from certain medications or medical conditions) may have a higher risk of SCC and more aggressive behavior.
A personal history of skin cancer raises the chance of developing another.
Family History and Genetics
Genetics plays a role in some cases. A family history of melanoma or certain inherited syndromes can raise risk, and
the National Cancer Institute notes that multiple genes and hereditary syndromes are associated with different skin
cancers. If skin cancer runs in your familyespecially multiple melanomas or early-onset casestell your clinician.
How Dermatologists Evaluate a Suspicious Skin Neoplasm
A good evaluation usually includes:
- History: how long it’s been there, whether it’s changing, symptoms (itching, bleeding, pain), sun exposure, tanning history, immune status.
- Skin exam: a full look at the lesion and often a scan for other concerning spots.
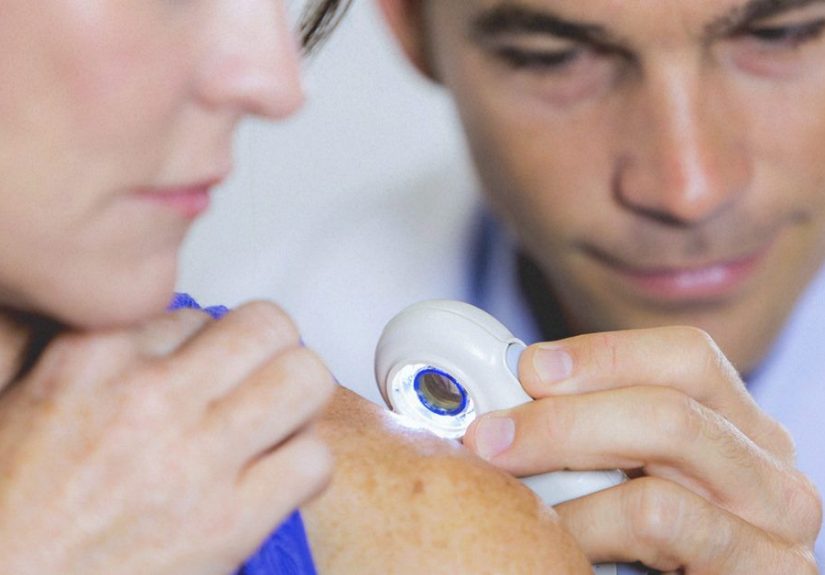
- Dermoscopy: a magnified, polarized view that can reveal patterns not visible to the naked eye.
- Biopsy: the key step when cancer is a possibility.
Biopsy Basics (Without the Drama)
A skin biopsy removes part or all of a lesion so it can be examined under a microscope. Common
types include shave biopsy, punch biopsy, and excisional biopsy. Which one is chosen depends on the lesion type,
location, and the specific question being asked (for example, “Is this melanoma?”).
If Melanoma Is Diagnosed: Staging May Include Lymph Node Evaluation
For certain melanomas, staging can include a sentinel lymph node biopsy to check whether cancer has
spread to nearby lymph nodes. Not everyone needs this, and decisions are individualizedbut it’s one example of how
diagnosis can guide next steps.
ABCDE and Other Warning Signs You Can Use at Home
Dermatologists often teach the ABCDE rule for spotting potential melanomas:
- Asymmetry: one half doesn’t match the other
- Border: irregular, scalloped, or poorly defined edges
- Color: varied colors (tan, brown, black, red, white, blue)
- Diameter: often > 6 mm (but smaller melanomas exist)
- Evolving: changing in size, shape, color, or symptoms
Also watch for the “ugly duckling” sign: a spot that looks different from your other moles.
And remember: non-melanoma skin cancers can look like a non-healing sore, a crusty patch, or a persistent bump that
bleeds easily.
Prevention and Risk Reduction That Actually Helps
No prevention plan is perfect, but proven strategies stack the odds in your favor:
- Avoid indoor tanning.
- Use sun-protective clothing, hats, and sunglasses.
- Seek shade, especially when UV is strong.
- Use broad-spectrum sunscreen as part of a bigger plan (and reapply as directed).
- Do regular self-checks and get clinician exams if you’re high risk or notice changes.
One helpful nuance: some cancer-prevention evidence varies by cancer type. For example, major cancer resources note
that sunscreen prevents sunburn and is recommended as part of sun safety, while evidence questions remain in certain
areas (like melanoma prevention specifically). The practical takeaway is simple: don’t rely on sunscreen alone.
Combine it with shade and clothing for the best protection.
When to See a Dermatologist (Sooner Rather Than Later)
Make an appointment if you notice:
- A new spot that grows quickly or looks unusual
- A mole that changes (especially ABCDE changes)
- A sore that doesn’t heal within a few weeks
- Bleeding, crusting, or persistent tenderness without a clear cause
- A lesion labeled “uncertain behavior” that needs next-step planning
If you’re told a lesion is benign, ask what to watch for and whether photos or follow-up exams are recommended.
If you’re told it’s malignant, ask about treatment options and follow-up schedule. If you’re told it’s uncertain,
ask: “What’s the plan to get certainty?”
Medical note: This article is for general education and does not replace professional medical advice. If you
have a concerning lesion, seek evaluation by a qualified healthcare professional.
Real-World Experiences (Common Stories People Share) 500+ Words
When people talk about skin neoplasms, the medical terms are only half the story. The other half is what it feels
like to live through the discovery, the waiting, and the decisions. And while every case is different, a few themes
show up again and again.
First: most people don’t notice a “classic” warning sign. A lot of benign growths are found
accidentallysomeone catches a “stuck-on” brown spot while changing a shirt, or a partner points out a bump on the
back that’s been quietly existing for months. People often describe a moment of surprise followed by a mental
spiral that goes something like: “It’s probably nothing… unless it’s everything.”
Second: uncertainty is emotionally louder than the lesion itself. Many skin neoplasms don’t hurt.
They just exist. But once a clinician says “we should biopsy that,” the spot suddenly becomes the main
character in your life. People commonly say the waiting period between biopsy and results feels longer than it is,
even if it’s only a few days. This is especially true for “uncertain behavior” resultsbecause the mind hates
unfinished sentences. If you’ve ever refreshed a tracking page for a package you didn’t even need, you understand
the vibe.
Third: pathology language can be confusing on purpose (in a good way). People often assume a report
must be either “benign” or “cancer.” Then they see words like “atypical,” “cannot exclude,” or “uncertain malignant
potential,” and it feels like the report is speaking in riddles. In reality, many of these phrases reflect careful,
responsible medicine. Patients frequently describe relief when a dermatologist explains, in plain language, that
“uncertain behavior” often means “we need a bigger sample to be sure,” not “we found secret cancer hiding in the
wallpaper.”
Fourth: the treatment experience is often less dramatic than people fear. For common cancers like
basal cell or squamous cell carcinoma, people often report that the most stressful part was the anticipation. Once
they understand the planwhether that’s a simple excision, a topical treatment, or a specialized procedurethe
process feels manageable. They also tend to say the follow-up routine becomes empowering: regular checks, better sun
habits, and a sharper eye for what’s “normal” on their own skin.
Fifth: lifestyle changes are real, but they’re usually practical. After a scare (or diagnosis),
people commonly stop “optimizing” for a tan and start optimizing for consistency: sunscreen by the front door, a hat
that actually gets worn, sun-protective clothing for long outdoor days, and phone photos of moles they want to
track. The biggest shift is often not perfectionit’s repetition. Many people say they didn’t become a new person;
they just became the version of themselves who re-applies sunscreen and doesn’t negotiate with noon sunlight.
Finally: reassurance matters, but so does vigilance. People who’ve had a benign diagnosis often
describe a lingering worry that the next spot could be worse. Over time, most find a healthier balance: they don’t
panic about every freckle, but they also don’t ignore changes. That “middle lane” is the goalcalm attention, not
constant fear. If you take anything from real-world experiences, let it be this: you don’t need to diagnose your
skin at home. You just need to notice it, respect change, and get help when something feels off.
Conclusion
“Skin neoplasm” is a wide umbrella that covers harmless growths, precancerous changes, and true skin cancers.
Understanding the behavior categoriesbenign, malignant, and
uncertain behaviorhelps you interpret medical language without jumping to worst-case conclusions.
The smartest approach is a mix of awareness (ABCDE + “ugly duckling”), practical prevention (no tanning beds, sun
protection habits), and timely evaluation when something changes. Your job isn’t to become a dermatologist.
Your job is to be the person who noticesand actsbefore a small problem becomes a big one.




