Table of Contents >> Show >> Hide
- What osteoarthritis actually is (and why it acts like a grumpy hinge)
- Home remedies that pull real weight (not just “good vibes”)
- 1) Heat and cold therapy: simple, cheap, oddly powerful
- 2) Joint-friendly movement: the “motion is lotion” principle
- 3) Strength training: protect the joint by building its bodyguards
- 4) Weight management (if needed): the “force multiplier” you can’t ignore
- 5) Supportive gear: braces, sleeves, shoe inserts, and the underrated cane
- 6) Topical relief at home: creams and gels that don’t involve a whole-body side quest
- 7) Sleep, stress, and pacing: boring… until you try it and it works
- 8) Anti-inflammatory eating patterns: less hype, more helpful habits
- Supplements and complementary options: what’s worth a look (and what needs a reality check)
- Evidence-based medical treatments (the “use the toolbox” approach)
- How to build your personal OA plan (without turning your life into a spreadsheet)
- When to call a professional (don’t tough it out in the name of pride)
- Conclusion: the best OA “home remedy” is consistency (sorry, it’s true)
- Experiences: what living with osteoarthritis often looks like in real life (and what tends to help)
- SEO tags (JSON)
Quick note before we get cozy: osteoarthritis (OA) is common, stubborn, and wildly unimpressed by “one weird trick.” The good news? A smart mix of home remedies and evidence-based medical treatments can meaningfully cut pain, improve movement, and help you feel more in charge of your joints. This article is for general educationif you have severe pain, sudden swelling, fever, a hot/red joint, or trouble bearing weight, check in with a clinician.
What osteoarthritis actually is (and why it acts like a grumpy hinge)
Osteoarthritis is a wear-and-repair problem that happens in joints over time. The cartilage that helps bones glide can thin, the bone underneath can change, and the joint lining may get irritated. The result is the classic OA combo platter: pain with activity, stiffness after sitting (often shorter than 30 minutes), reduced range of motion, and occasional swelling.
OA isn’t just “old age.” Past injuries, repetitive strain, genetics, body weight, muscle weakness, and joint alignment all play roles. Translation: there are multiple levers you can pullmany of them at hometo calm symptoms and protect function.
Home remedies that pull real weight (not just “good vibes”)
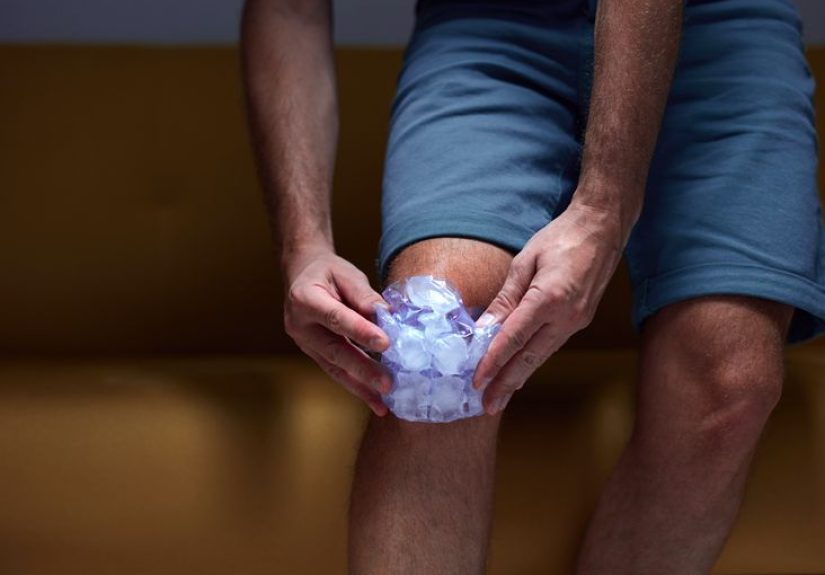
1) Heat and cold therapy: simple, cheap, oddly powerful
Think of heat as the “morning loosener” and cold as the “after-activity calmer.” Heat can relax tight muscles and reduce that rusty-joint feeling. Cold can numb sharp pain and dial down swelling after you’ve overdone it (or when your knee is throwing a tantrum).
- Heat ideas: warm shower, heating pad, warm towel, warm bath, paraffin wax for hands (if recommended).
- Cold ideas: gel pack, bag of frozen peas (the MVP of freezers everywhere), wrapped in a thin towel.
Pro tip: Try heat in the morning for stiffness, and cold later if the joint feels puffy or irritated. Your body gets the final voteuse what helps.
2) Joint-friendly movement: the “motion is lotion” principle
When OA hurts, the natural instinct is to move less. Unfortunately, less movement can lead to stiffer joints and weaker muscles, which often increases pain over time. Gentle, consistent activity helps by improving circulation, strengthening the joint’s support system, and keeping your range of motion from shrinking.
Good options (choose what you’ll actually do):
- Walking (shorter, more frequent walks beat one heroic march)
- Cycling (stationary bikes are great for predictable, low-impact control)
- Swimming or water aerobics (buoyancy = less joint load)
- Yoga or mobility work (gentle range-of-motion, not circus tricks)
- Tai chi (slow, controlled movement + balance training)
If you’re thinking, “Sure, but exercise hurts,” you’re not alone. A little discomfort can be normal when you’re startingsharp pain that lingers or worsens is your cue to scale back and talk with a pro (physical therapist is ideal).
3) Strength training: protect the joint by building its bodyguards
Muscles act like shock absorbers. When the muscles around a joint are stronger, the joint often hurts less because it’s not taking the full force of every step, squat, and stair climb. For knee OA, strengthening the thighs and hips can be especially helpful. For hand OA, grip and finger exercises can maintain function.
Easy starters: sit-to-stand from a chair, step-ups on a low step, gentle resistance band work, wall push-ups, and calf raises. You don’t need a gymjust consistency and good form.
4) Weight management (if needed): the “force multiplier” you can’t ignore
For weight-bearing joints (knees, hips, spine), extra body weight increases joint stress. Even modest weight loss can reduce symptoms and make movement easier. This isn’t about chasing a lookit’s about lowering mechanical load and inflammation signals that can amplify pain.
If weight loss is a goal, aim for sustainable changes: smaller portions, more protein and fiber, fewer ultra-processed snacks that mysteriously vanish at 11 p.m., and more daily movement. If dieting has been a rough ride in the past, ask a clinician about realistic options and support programs.
5) Supportive gear: braces, sleeves, shoe inserts, and the underrated cane
Supportive devices can reduce stress on painful joints and make daily activities easier. A knee brace or sleeve may improve stability and confidence. Shoe inserts can help alignment (especially if you have flat feet or uneven wear patterns). A cane can take meaningful pressure off a hip or kneeyes, even if you feel “too young” for it. Your joint does not care about your aesthetic. Your joint cares about leverage.
6) Topical relief at home: creams and gels that don’t involve a whole-body side quest
Topical options deliver relief right where you need it and can reduce systemic side effects compared with pills. Common categories include:
- Topical NSAIDs (often first-line for knee/hand OA)
- Capsaicin (a “warm/tingly” ingredient that can reduce pain signals over time)
- Counterirritants (menthol/camphor-style cooling or warming sensations)
If you try capsaicin, wash hands thoroughly and keep it away from eyes (unless you enjoy living dangerously, which we do not recommend).
7) Sleep, stress, and pacing: boring… until you try it and it works
Pain and poor sleep feed each other like two raccoons raiding the same trash can. Improving sleep hygiene (regular schedule, less late caffeine, calming wind-down routine) can reduce pain sensitivity. Stress also amplifies pain perception, so relaxation techniquesbreathing exercises, guided imagery, mindfulness, gentle stretchingcan be surprisingly useful.
Pacing matters too: alternate activity with rest, break chores into smaller sessions, and avoid the “I feel good so I’ll do everything today” trap that leads to tomorrow’s regret.
8) Anti-inflammatory eating patterns: less hype, more helpful habits
No diet “cures” OA, but eating patterns that support overall health can help with weight management, energy, and inflammation-related pain sensitivity. Many people do well with a Mediterranean-style pattern: fruits, vegetables, beans, whole grains, olive oil, nuts, and fishplus less added sugar and fewer ultra-processed foods.
If you notice certain foods clearly worsen your symptoms (some people report issues with high-sugar foods or excessive alcohol), it’s reasonable to experiment carefullyone change at a timeso you can see what’s real and what’s coincidence.
Supplements and complementary options: what’s worth a look (and what needs a reality check)
Glucosamine and chondroitin: mixed evidence, not a guaranteed win
These supplements are popular because they’re components of cartilage, and the logic sounds neat: “If cartilage is the problem, let’s feed the cartilage.” Research has been mixed. Some people report symptom improvement; many feel no difference. If you try them, talk to a clinician firstespecially if you take blood thinners or have chronic conditionsand give it a fair trial period, then stop if there’s no benefit.
Turmeric/curcumin, ginger, omega-3s: modest help for some
Some supplements have anti-inflammatory properties and may slightly reduce pain for certain people. The big caution is quality and interactions: supplements aren’t regulated like prescription medications. Choose reputable brands (third-party testing when possible) and review safety with your healthcare teamespecially if you take anticoagulants, have gallbladder issues, or are preparing for surgery.
Acupuncture, massage, tai chi: low-risk options that may improve pain and function
Mind-body and physical approaches can be helpfulespecially when paired with a strong movement plan. Tai chi is often highlighted for knee and hip OA because it builds balance, strength, and confidence. Massage may provide short-term relief for stiffness and muscle tension. Acupuncture may help some people with pain.
Evidence-based medical treatments (the “use the toolbox” approach)
Home remedies are powerful, but OA often benefits from combining self-care with targeted medical treatments. Here are common options clinicians use, generally moving from lower risk to higher intensity.
1) Physical therapy (PT): a customized plan, not generic “do more walking” advice
PT can help you strengthen the right muscles, improve joint mechanics, and learn how to move without provoking flare-ups. A good physical therapist also teaches pacing strategies, safe progressions, and ways to modify daily activities (stairs, lifting, kneeling, typing) so you keep living your life instead of negotiating with your knee for permission.
2) Medications: topical first, then oral when appropriate
- Topical NSAIDs: Often recommended early for knee (and sometimes hand) OA because they can reduce pain with fewer whole-body side effects than oral NSAIDs.
- Oral NSAIDs: Effective for many people, but they carry risks (stomach bleeding/ulcers, kidney issues, and increased cardiovascular risk in some individuals). They should be used thoughtfullyespecially in older adults or those with heart, kidney, or GI history.
- Acetaminophen: Can help mild pain for some people, but it must be used safely. Too much can harm the liver. Many clinical resources advise staying under 3,000 mg/day unless a clinician directs otherwise, and even less if you have liver disease or drink alcohol regularly.
- Duloxetine: A prescription medication that can help chronic musculoskeletal pain (including OA-related pain) for some patientsparticularly when pain affects mood, sleep, or daily function.
About opioids: For OA, most guidelines discourage routine opioid use because benefits are limited and risks are significant. In specific situations, tramadol may be considered, but typically only when other options aren’t workable.
3) Joint injections: short-term relief for the right person
Injections aren’t magic, but they can be usefulespecially when pain is blocking rehab and movement (which are long-term essentials).
- Corticosteroid injections: Often provide pain relief for weeks (sometimes longer). Clinicians usually limit how many you get in a year because repeated injections may have downsides for joint tissues.
- Hyaluronic acid (“gel”) injections: Evidence is mixed. Some people report relief; some guidelines do not recommend them routinely for knee OA, while certain clinicians may still consider them case-by-case.
4) When conservative care isn’t enough: surgical options
If OA becomes severepersistent pain, major function loss, poor sleep, inability to work or do daily taskssurgery may enter the chat. Options include joint replacement (most commonly knee or hip) and, less commonly, other procedures depending on the joint and anatomy. Surgery is typically considered after a solid trial of non-surgical care, but the timing is personal and depends on quality of life.
How to build your personal OA plan (without turning your life into a spreadsheet)
If you want the simplest effective structure, think in three layers:
- Daily foundations: joint-friendly movement, basic strength work, heat/cold, pacing, and sleep routines.
- Targeted symptom tools: topical relief, braces/insoles, and short courses of meds when appropriate.
- Clinician-guided upgrades: PT, injections, andif neededsurgical consultation.
Keep a tiny symptom log for 2 weeks. Note what you did and how you felt. Not forever. Just long enough to spot patterns: “Long car rides wreck my hip,” “Stairs are my villain,” “Water aerobics makes my knee feel oddly optimistic.” That information helps you and your clinician choose smarter interventions.
When to call a professional (don’t tough it out in the name of pride)
- Sudden severe pain, major swelling, redness/warmth, or fever
- Joint locking, giving way, or inability to bear weight
- Pain that disrupts sleep for weeks
- New numbness/weakness, or pain after a fall/injury
- You’re relying on pain meds frequently just to function
Conclusion: the best OA “home remedy” is consistency (sorry, it’s true)
Osteoarthritis care works best when you stop hunting for a single perfect fix and start using a practical combination: heat/cold, movement, strengthening, smart pacing, and supportive devicesthen add medical treatments like topical/oral meds, PT, or injections when needed. OA is a long game, but small daily choices often stack into big wins: fewer flare-ups, better mobility, and more control over your day.
Experiences: what living with osteoarthritis often looks like in real life (and what tends to help)
People often describe osteoarthritis as a “predictable surprise.” Predictable because the same joint complains in familiar situationsstairs, long walks, cold mornings, long drives. Surprising because the intensity can change day to day, sometimes for reasons that feel unfairly random. A common experience is waking up with stiffness that makes you move like a folding chair being opened for the first time. Many people find that heat in the morning helps them “start the engine,” especially for hands, hips, and knees. A warm shower, a heating pad, or gentle mobility movements can reduce that first-wave stiffness enough to make breakfast and basic chores feel possible again.
Another shared experience is the “too much, too soon” cycle. Someone has a decent day, feels encouraged, and decides to clean the entire house, run errands, and finally reorganize the garage (because apparently today is the day they become a superhero). The next day, the joint responds with a firm memo: absolutely not. People who do best long term often learn pacingnot as giving up, but as playing strategy. They split tasks into smaller chunks, schedule breaks before pain spikes, and rotate activities so the same joint isn’t stressed for hours. This can feel annoyingly slow at first, but it often prevents multi-day flare-ups that steal time anyway.
Many individuals report that strengthening was the turning pointnot because it eliminated OA, but because it changed how the joint behaved under load. For knee OA, people commonly notice that stronger thighs and hips make stairs less dramatic. For hip OA, building glute strength often improves walking tolerance. For hand OA, gentle grip and finger exercises can make daily tasksopening jars, typing, cookingfeel less like a negotiation. What surprises many is that the “right” exercises are often simple. Progress usually comes from doing small, manageable sessions consistently rather than chasing intense workouts. People frequently mention that working with a physical therapist helped them stop guessing and start progressing safely.
Heat and cold show up in real-life routines more than fancy gadgets. A lot of people become loyal to ice packs after activityespecially if swelling is part of their patternwhile using heat for stiffness and muscle tightness. Some alternate both: heat to loosen up, movement to get going, and cold later if the joint feels irritated. Topical treatments are another common favorite because they’re targeted and don’t feel like “taking another pill.” People often experiment with topical NSAIDs, menthol-based gels, or capsaicinthen keep whatever helps and ditch the rest. The most consistent feedback is that these tools work best as part of a broader plan, not as stand-alone saviors.
Finally, many people talk about the emotional sidefrustration, worry about getting worse, and the mental fatigue of chronic discomfort. Those who feel most stable often build a support system: a clinician who listens, a PT who teaches, friends or family who understand boundaries, and a routine that includes stress-lowering practices (even short breathing exercises or a calm evening walk). In real life, success often looks less like “pain-free forever” and more like “I can do more of what I care about, with fewer flare-ups, and I recover faster when symptoms spike.” That’s a meaningful winand it’s exactly what a good osteoarthritis plan is aiming for.