Table of Contents >> Show >> Hide
- First, a quick translation: “mouth sore” is a category, not a diagnosis
- What a canker sore usually looks and feels like
- What oral cancer sores and warning signs can look like
- Canker sore vs. cancer: a practical comparison
- The “two-week rule”: when to stop guessing and get checked
- “If it’s not a canker sore, what else could it be?”
- Why do canker sores happen?
- What you can do at home for an uncomplicated canker sore
- How clinicians check for oral cancer (and why that’s a good thing)
- Risk factors: who should be extra alert?
- How to lower your risk (without living in fear)
- Real-life experiences: what people commonly go through (and what helps)
- Bottom line
Your mouth is basically a high-traffic intersection: hot coffee, crunchy chips, spicy salsa, braces, toothbrush bristles,
accidental cheek bites… and that’s before stress shows up and starts throwing chairs. So when a sore appears, it’s normal to wonder:
“Is this just a canker sore… or something scarier?”
Here’s the reassuring truth: most mouth sores are harmless and heal on their own. But a small number of mouth sores (or mouth changes)
can be warning signs of oral cancer or throat (oropharyngeal) cancerespecially when they don’t heal or come with other red flags.
This guide breaks down what to look for, what’s usually benign, what deserves a closer look, and when to stop Googling and call a dentist or doctor.
First, a quick translation: “mouth sore” is a category, not a diagnosis
“Mouth sore” can mean a lot of things: a canker sore (aphthous ulcer), a cold sore (herpes), a burn from pizza cheese that lava-slid onto your palate,
a rough spot from a sharp tooth, irritation from dentures, a fungal infection (thrush), or inflammation from conditions like lichen planus.
Oral cancer can also start as a sore or patchbut it tends to behave differently over time. The biggest difference isn’t always how it looks on Day 1.
It’s what it does by Day 14 (and beyond).
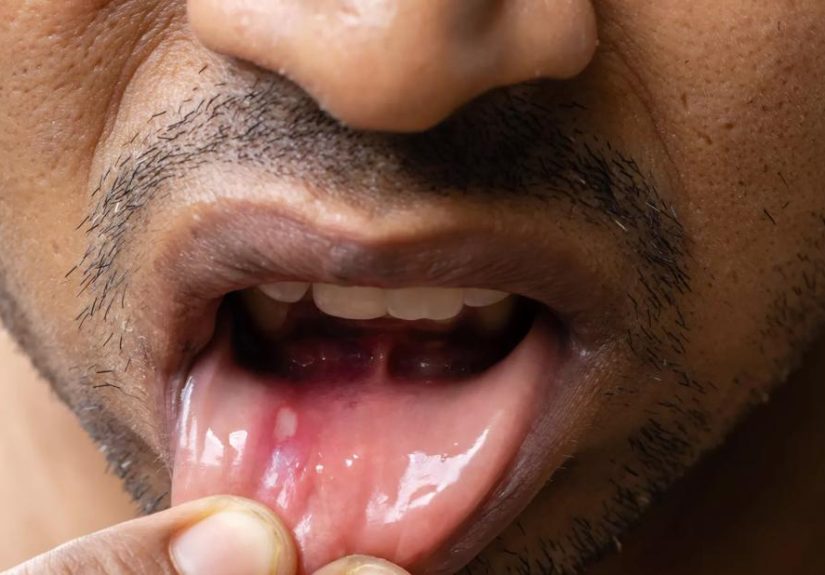
What a canker sore usually looks and feels like
Canker sores (also called aphthous ulcers) are small, shallow ulcers that typically show up on the soft tissues inside your mouth:
inner cheeks, inner lips, the tongue, or the soft area near the gums. They’re not contagious (unlike cold sores), and most heal in about
1–2 weeks.
Common canker sore clues
- Location: Usually inside the mouth (inner cheeks/lips, tongue, soft gum area).
- Shape and color: Often round/oval with a white, yellow, or gray center and a red border.
- Pain level: Often stings or burnsespecially with citrus, spicy foods, salty snacks, or toothpaste.
- Timeline: Peaks in discomfort early, then gradually improves and heals within two weeks.
- Pattern: May recur, especially with stress, mouth injury, or certain triggers.
Types of canker sores (yes, there are “models”)
- Minor: The most commonsmall and typically heals without scarring.
- Major: Larger, deeper, more painful; can take longer to heal and may scar.
- Herpetiform: Clusters of tiny ulcers that can mergedespite the name, they’re not caused by herpes.
If you get occasional canker sores that heal normally, it’s annoyingbut not usually dangerous. If you get severe, frequent, or unusually persistent
ulcers, that’s when it’s worth checking for underlying issues (more on that below).
What oral cancer sores and warning signs can look like
Oral cancer doesn’t always announce itself with dramatic pain. Early changes can be subtle: a sore that won’t heal, a persistent rough patch,
a lump, or a red/white area that doesn’t go away. Throat (oropharyngeal) cancers can show up as persistent sore throat, trouble swallowing,
or a lump in the neck.
Common warning signs to take seriously
- A mouth sore that doesn’t heal (or doesn’t clearly improve) after about 2 weeks.
- A lump, thickening, or raised area in the mouth, cheek, jaw, or neck.
- White or red patches (sometimes called leukoplakia or erythroplakia) that persist.
- Unexplained bleeding, numbness, or persistent pain.
- Trouble chewing, swallowing, speaking, or moving the jaw/tongue.
- Loose teeth or dentures that suddenly don’t fit right.
- Ear pain that doesn’t resolve (especially on one side) along with other symptoms.
Not every persistent sore is cancer. But cancer is one of the reasons clinicians take “doesn’t heal” seriouslybecause that’s the pattern
that deserves a professional look.
Canker sore vs. cancer: a practical comparison
These aren’t perfect rules (bodies love exceptions), but this checklist can help you decide whether you’re likely dealing with a typical
canker soreor something that needs evaluation.
| Feature | Typical Canker Sore (Aphthous Ulcer) | Possible Cancer Red Flag |
|---|---|---|
| Healing time | Usually resolves in 7–14 days | Persists beyond 2 weeks or keeps returning in the same spot |
| Location | Inside mouth (cheeks, lips, tongue, soft gums) | Anywhere, including lips; may be a persistent patch/ulcer in one area |
| Pain | Often painful/stinging | May be painless early; pain isn’t a reliable “yes/no” clue |
| Appearance | Small, round/oval, white/yellow center with red rim | Non-healing ulcer, persistent red/white patch, firm or raised area |
| Other symptoms | Mostly local discomfort | Lump in neck, swallowing trouble, voice changes, numbness, unexplained bleeding |
The “two-week rule”: when to stop guessing and get checked
A helpful rule of thumb used by many clinicians: if a mouth sore, ulcer, or patch lasts longer than about two weeksor fails to clearly improveschedule an exam.
Dentists and primary care clinicians see mouth sores all the time, and they’re trained to spot which ones are ordinary and which ones need testing.
Book an appointment sooner (not later) if you notice:
- A sore that’s getting bigger, deeper, or more irregular.
- A firm lump, thickened area, or swelling that doesn’t go down.
- Persistent red or white patches.
- New numbness, persistent bleeding, or unexplained pain.
- Difficulty swallowing, chewing, or moving the tongue/jaw.
- A neck lump or swollen lymph node that lasts more than two weeks.
If you have a sore plus major symptoms (like trouble breathing, severe swelling, or you can’t swallow fluids), treat it as urgent.
“If it’s not a canker sore, what else could it be?”
Mouth sores have a surprisingly crowded “look-alike” list. Here are a few common culprits that can mimic (or trigger) canker sores:
1) Trauma and irritation
Biting your cheek, a sharp tooth edge, aggressive flossing, new braces, dentures, retainers, or rough dental work can cause a sore spot
that feels suspiciously dramatic. These often improve once the irritation stops.
2) Cold sores (HSV-1)
Cold sores often appear on or near the lip border and are caused by a virus. They can form clusters of blisters and are contagious.
Canker sores usually occur inside the mouth and are not contagious.
3) Burns and food injuries
Hot foods can burn the palate, and sharp foods (hello, tortilla chips) can scrape tissue. These can look like ulcers but usually have a clear “oops” moment behind them.
4) Infections (like thrush)
Oral thrush can cause tender areas and white patches. It’s more common after antibiotics, with inhaled steroids, or with immune changes.
5) Inflammatory conditions
Some chronic conditions can involve the mouth (for example, lichen planus or autoimmune/inflammatory disorders). If sores are frequent, severe,
or come with other symptoms (GI issues, joint pain, skin changes), it’s worth mentioning to a clinician.
Why do canker sores happen?
The frustrating answer is: we don’t always know. But several triggers are commonly associated with outbreaks:
- Minor mouth injury: biting the cheek, toothbrush trauma, dental work.
- Stress and poor sleep: your immune system notices when you’re running on fumes.
- Certain foods: acidic foods (citrus, tomatoes), spicy foods, crunchy/salty snacks.
- Nutrient deficiencies: iron, folate, vitamin B12 can play a role for some people.
- Underlying conditions: severe or recurrent cases sometimes warrant evaluation for systemic issues.
If you’re getting frequent, severe ulcersor ulcers that behave oddly (very large, long-lasting, scarring, or accompanied by other symptoms)
ask about a deeper workup. Sometimes the mouth is the first place your body posts a “maintenance required” sign.
What you can do at home for an uncomplicated canker sore
If the sore looks and behaves like a typical canker sore (and you’re otherwise well), comfort care is usually the name of the game.
Think: reduce irritation, reduce pain, support healing.
Comfort moves that actually help
- Rinse gently: salt water or baking soda rinses can soothe irritation (spit, don’t swallow large amounts).
- Protect it: OTC protective pastes or patches can reduce friction while you eat and talk.
- Numb the pain: topical anesthetics can take the edge off before meals.
- Choose “soft and boring” foods: yogurt, smoothies, eggs, oatmealthis is not the time for extra-hot wings.
- Use a soft toothbrush and avoid poking the sore like it owes you money.
When home care isn’t enough
If pain is severe or sores are frequent, clinicians may recommend prescription rinses or topical anti-inflammatory medicines.
The goal is symptom control and faster healingespecially when sores interfere with eating, speaking, or sleep.
How clinicians check for oral cancer (and why that’s a good thing)
An evaluation doesn’t mean someone thinks you “definitely have cancer.” It means the sore has crossed the threshold where a professional exam is smart.
Clinicians will look at the sore, ask about timeline and risk factors, and examine nearby tissues and lymph nodes.
If something looks suspicious or persists, the next step may be referral to a specialist and possibly a biopsy (a small tissue sample).
A biopsy is the only way to confirm whether a lesion is cancerous or not. The upside: catching oral cancer early greatly improves treatment outcomes.
Risk factors: who should be extra alert?
Oral cancer can happen to anyone, but risk goes up with certain exposures and conditions. Key risk factors include:
- Tobacco use (smoking or smokeless tobacco)
- Heavy alcohol use (and the combination of tobacco + alcohol increases risk more)
- Excess sun exposure (especially for lip cancer)
- HPV infection (a major risk factor for many oropharyngeal cancers)
- Weakened immune system
- Age (risk increases with age, though HPV-related throat cancers may appear in younger adults)
One important note: HPV-related cancers often involve the tonsils and back of the tongue/throat rather than classic “front of mouth” lesions.
That’s why symptoms like persistent sore throat, swallowing trouble, or a neck lump deserve attention too.
How to lower your risk (without living in fear)
You don’t need to treat every mouth sore like a crisis. You do need a plan.
A calm, practical prevention checklist
- Don’t use tobacco. If you already do, quitting is one of the biggest risk reducers you can choose.
- Limit alcohol and avoid the tobacco + heavy alcohol combo.
- Protect your lips from sun with SPF lip balm, especially outdoors.
- Stay current on HPV vaccination if you’re eligible (it helps prevent HPV-related cancers).
- Keep regular dental visits. Oral cancer screenings can be part of routine exams.
- Don’t ignore “persistent.” If it doesn’t heal in two weeks, get it checked.
Real-life experiences: what people commonly go through (and what helps)
If you’ve ever had a mouth sore, you know it has a special talent: it makes you hyper-aware of your tongue, your teeth, and your own thoughts.
Many people describe the same emotional arcfirst annoyance, then suspicion, then full-on detective mode in the bathroom mirror with a flashlight.
A very common story starts with a totally ordinary trigger. Someone bites their cheek while chewing, or a tortilla chip lands a sharp hit,
or a braces wire starts rubbing like it’s trying to file a complaint. The sore shows up the next day, and suddenly every meal feels like a reality show challenge:
“Today’s task: eat a sandwich without wincing.” In these cases, the sore often improves once the irritation stopsand that improvement is a comforting clue.
Another common experience is “the stress flare.” People notice canker sores popping up during exam weeks, work deadlines, family drama,
or when sleep gets sloppy. The sore becomes the body’s tiny, rude reminder that stress doesn’t just live in your calendarit can show up in your mouth.
For many, simply returning to regular sleep, hydration, and less acidic/spicy food makes the next few days more tolerable.
Then there’s the worry spiral, which often sounds like: “It’s been 10 days… is it supposed to be gone yet?”
What helps here is using a simple tracking approach instead of anxious guesswork. Many people find it calming to take a quick photo on Day 1,
then again every couple days in similar lighting. The goal isn’t obsessionit’s clarity. If it’s shrinking and less painful, that’s reassuring.
If it’s not changing, or it’s getting worse, you have solid information to bring to a dentist or doctor.
Some people notice patterns with food triggerscitrus, pineapple, spicy sauces, very salty snacks, or rough foods like crusty bread.
They’ll often switch to “soft and boring” meals for a week and use topical relief before eating. It’s not glamorous, but it’s effective.
Others realize their sore keeps showing up in the exact same spot because a tooth edge or dental appliance is scraping that area.
In those situations, a dental adjustment can be the real solutionbecause no mouth tissue enjoys being repeatedly ambushed.
People also describe the relief of getting checked when something feels off. The appointment itself is usually quick: a clinician looks, asks about timing,
checks surrounding tissue, and explains whether it looks like a typical ulcer, irritation, infection, or something that needs follow-up.
Even when the outcome is “this looks benign,” the reassurance can be huge. And when the outcome is “let’s investigate,” early evaluation is a giftnot a punishment.
It’s how problems get found when they’re most treatable.
The most useful mindset shift is this: you don’t have to choose between ignoring symptoms and panicking about them.
You can treat your mouth like you’d treat any other body partwatch for changes, respect the timeline, and get help when something doesn’t heal.
That’s not alarmist. That’s just smart.
Bottom line
Most mouth sores are canker sores or minor irritation and heal within 1–2 weeks. Oral cancer is less common, but it’s important because it can start subtly.
The biggest “serious” clue is persistence: a sore, patch, or lump that doesn’t heal or improve after two weeks, especially if it comes with
swallowing trouble, a neck lump, unexplained bleeding, numbness, or voice changes. When in doubt, get it checked. Peace of mind is a valid medical outcome.