Table of Contents >> Show >> Hide
- Why Your Body Waves the White Flag
- 1. You’re Tired All the Time, Even After Rest
- 2. Your Sleep Is a Mess
- 3. Your Head, Neck, or Jaw Always Feel Tight
- 4. Your Gut Has Entered the Group Chat
- 5. You Have Brain Fog and Can’t Focus
- 6. You’re Irritable, Snappy, or Weirdly Emotional
- 7. You Keep Getting Sick or You Never Fully Bounce Back
- 8. Your Heart Feels Like It’s Doing Too Much
- 9. Your Body Aches More and Recovers More Slowly
- 10. You’ve Lost Interest in Things That Normally Feel Good
- What Slowing Down Actually Looks Like
- When to Get Checked Out
- Real-Life Experiences: What This Can Feel Like Day to Day
- Conclusion
- SEO Tags
Some people get a polite nudge from their body when life is moving too fast. Other people get a full marching band: headaches, lousy sleep, random crying over a missing sock, and the strange feeling that even answering one more text might qualify as an extreme sport. If that sounds familiar, your body may be asking for something radical in modern life: a little less chaos and a little more recovery.
Slowing down does not mean quitting your job, moving to a cabin, and becoming emotionally available to mushrooms. It means noticing the signals your nervous system, muscles, gut, brain, and mood are already sending you. Chronic stress, poor sleep, nonstop stimulation, overtraining, and lack of recovery can pile up quietly. Then one day your body says, “Cool, I’ll handle this myself,” and suddenly everything feels harder than it should.
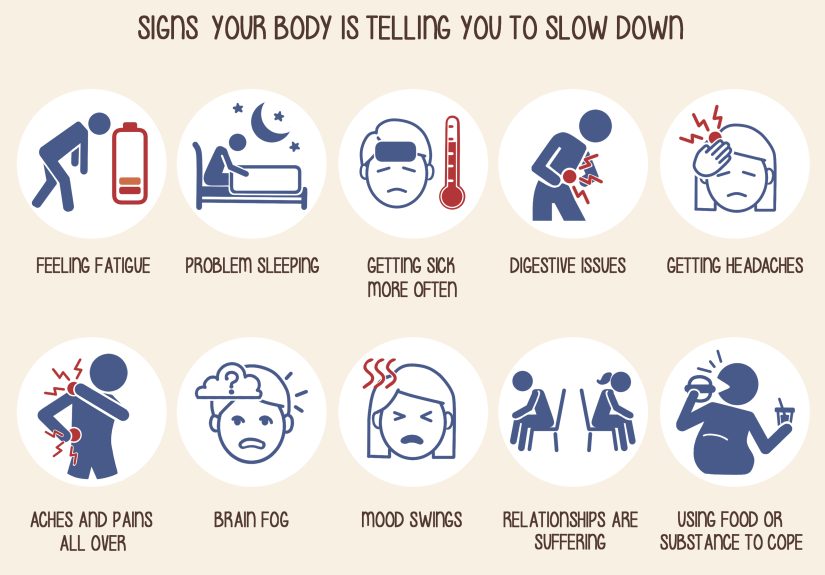
Below are 10 common signs your body is begging you to slow down, plus practical steps you can take right now. None of these signs automatically mean stress is the only cause. They can overlap with medical conditions, so think of this list as a smart starting point, not a diagnosis machine in blog form.
Why Your Body Waves the White Flag
When stress sticks around too long, your body does not stay in “helpful emergency mode.” Instead, the constant pressure can affect sleep, focus, digestion, muscle tension, energy, mood, and even how often you get sick. Add too little rest, too much caffeine, intense workouts without recovery, or a packed schedule with zero breathing room, and your body may start flashing warning lights long before you feel “burned out” in the dramatic movie-trailer sense.
1. You’re Tired All the Time, Even After Rest
Normal tiredness says, “I had a long day.” Recovery-deprived tiredness says, “I slept, but somehow I woke up feeling like a haunted charging cable.” If you feel drained most days, need heroic amounts of caffeine to function, or hit an energy wall by midmorning, your system may be overloaded.
What it can look like
You wake up unrefreshed, you drag through meetings, and small tasks feel weirdly physical. Even fun plans can sound exhausting. That is often a clue that your body is not getting enough real restoration, not just time in bed.
What to do
Protect the basics first: aim for a consistent sleep schedule, give yourself a wind-down routine, and stop treating bedtime like a casual suggestion. Try reducing late-day caffeine, keeping your room cool and dark, and giving yourself 30 to 60 screen-light-free minutes before bed. If exhaustion is persistent, severe, or keeps getting worse, talk with a healthcare professional.
2. Your Sleep Is a Mess
Sometimes your body begs you to slow down by making sleep feel annoyingly complicated. You are tired but wired. You fall asleep, then wake up at 3 a.m. ready to mentally relive every awkward interaction since middle school. Or you sleep longer but still feel foggy and unrested.
What it can look like
Difficulty falling asleep, waking frequently, sleeping too little, oversleeping on weekends, or feeling groggy no matter how many hours you got. Stress and sleep tend to team up like unhelpful best friends: stress disrupts sleep, and poor sleep makes stress feel bigger.
What to do
Create a boringly consistent sleep routine. Go to bed and wake up around the same time, even on weekends. Keep naps short, avoid heavy meals and alcohol close to bedtime, and cut doom-scrolling before sleep. If snoring, breathing pauses, insomnia, or severe daytime sleepiness show up regularly, get checked out.
3. Your Head, Neck, or Jaw Always Feel Tight
Stress loves real estate in the head, neck, shoulders, and jaw. If you are getting more headaches, clenching your teeth, rubbing your temples, or carrying your shoulders somewhere near your ears, your body may be physically holding onto overload.
What it can look like
Tension headaches, neck stiffness, jaw soreness, shoulder tightness, or that end-of-day feeling that your upper back has been personally offended by your calendar.
What to do
Schedule short body resets before pain becomes your personality. Stand up every hour, unclench your jaw, stretch your chest and shoulders, and take a few slow breaths with a long exhale. Gentle exercise, hydration, posture changes, and reducing screen strain can help. But frequent headaches, sudden severe headache, neurologic symptoms, or chest-related symptoms should not be brushed off.
4. Your Gut Has Entered the Group Chat
Your digestive system is often one of the first places stress shows up. If your stomach flips before ordinary tasks, your appetite is all over the place, or your bathroom habits have become unpredictable, your body may be telling you it is not coping as smoothly as you think.
What it can look like
Upset stomach, nausea, bloating, constipation, diarrhea, reflux, stress-snacking, forgetting to eat, or feeling like your gut is conducting its own protest march.
What to do
Start with steady, simple habits: regular meals, enough water, less rushing while eating, and fewer “lunches” that are really just coffee plus denial. Walk after meals, limit alcohol if it is making symptoms worse, and track any patterns. Persistent pain, vomiting, black stools, blood in stool, or ongoing bowel changes deserve medical attention.
5. You Have Brain Fog and Can’t Focus
If your brain feels like it has 27 browser tabs open and one of them is playing music you cannot find, that counts. Sleep loss and ongoing stress can make it harder to focus, remember things, make decisions, and regulate emotions.
What it can look like
You reread the same email three times, forget why you walked into a room, struggle to finish familiar tasks, or feel mentally slower than usual. This is not a moral failure. It is often a recovery issue.
What to do
Lower cognitive clutter. Pick three priorities instead of ten. Use lists. Batch notifications. Build five-minute transition breaks between tasks instead of speed-running your day. If the fog is abrupt, severe, or paired with confusion, fainting, weakness, or speech changes, seek urgent care.
6. You’re Irritable, Snappy, or Weirdly Emotional
One of the sneakiest signs you need to slow down is emotional short-circuiting. Maybe you are more impatient, more reactive, or more likely to cry because the dishwasher beeped in a rude tone. When your stress load gets too high, your emotional buffer shrinks.
What it can look like
Short temper, restlessness, feeling overwhelmed, low frustration tolerance, resentment, or emotional numbness. You may also notice that tiny inconveniences feel enormous.
What to do
Do not just tell yourself to “be less dramatic.” That rarely works and is frankly lazy advice. Instead, reduce load where you can. Say no faster. Build quiet time into your day. Move your body. Talk to someone you trust. If distress is persistent or affecting relationships, work, or daily life, professional support can help a lot.
7. You Keep Getting Sick or You Never Fully Bounce Back
If every cold finds you, or you feel like your body is slower to recover from minor illnesses than it used to be, that is worth paying attention to. Chronic stress and poor sleep can chip away at how resilient you feel day to day.
What it can look like
Frequent sniffles, lingering fatigue after simple illnesses, feeling run-down more often, or taking longer than usual to feel normal again after a busy week.
What to do
Think less about “pushing through” and more about building capacity. Prioritize sleep, regular meals, hydration, movement, and actual rest days. Not fake rest where you answer emails horizontally. If infections are frequent or recovery feels unusually slow, check in with a clinician.
8. Your Heart Feels Like It’s Doing Too Much
Stress can show up as a racing heart, chest heaviness, shakiness, or that jittery adrenaline feeling when you are technically just sitting there answering a spreadsheet. Sometimes it is stress. Sometimes it is something more serious. Either way, listen.
What it can look like
Heart pounding, feeling on edge, chest tightness, shaky hands, or feeling revved up long after the stressful moment is over.
What to do
Pause before you power through. Sit down, loosen your shoulders, and try slow breathing with a longer exhale than inhale. Reduce stimulants if they are clearly worsening symptoms. But chest pain, shortness of breath, fainting, severe dizziness, or symptoms that feel intense or new should be evaluated urgently.
9. Your Body Aches More and Recovers More Slowly
When your system is overloaded, muscles often stop being cooperative. Workouts feel harder, soreness lasts longer, and even everyday tension can pile up into body aches. If you train hard without enough recovery, your body may start pushing back.
What it can look like
Lingering soreness, heavy legs, reduced performance, more aches than usual, trouble relaxing muscles, or feeling “fried” after routines that used to feel manageable.
What to do
Take recovery as seriously as effort. That means lighter days, easy walks, mobility work, adequate calories, hydration, and enough sleep. If you exercise intensely, watch for a pattern of worsening performance, irritability, poor sleep, and constant fatigue. Those are signs to back off, not double down out of spite.
10. You’ve Lost Interest in Things That Normally Feel Good
This is often the most important sign. When your body and brain need a slowdown, pleasure can flatten out. You stop enjoying hobbies, avoid people, feel detached, or move through the day on autopilot. The problem is not laziness. The problem is depletion.
What it can look like
You cancel plans you usually enjoy, feel disconnected from yourself, withdraw socially, or keep saying, “I’m fine, just busy,” while your joy quietly files a complaint.
What to do
Reduce nonessential commitments and add back small, low-pressure forms of pleasure: sunlight, music, a short walk, a real lunch break, a conversation with someone safe, or an hour without being reachable. If low mood, anxiety, numbness, or hopelessness stick around, professional mental health support is a strong move, not a dramatic one.
What Slowing Down Actually Looks Like
Slowing down is not one grand gesture. It is a collection of small decisions that tell your body it does not need to stay in emergency mode all day. That might mean going to bed on time, taking a real lunch break, scaling a workout from brutal to reasonable, turning off notifications for an hour, declining one commitment, or asking for help before you are hanging on by a paper clip.
A simple reset plan
- Sleep: Treat 7 or more hours as a health habit, not a luxury upgrade.
- Food: Eat regular meals with protein, fiber, and enough calories to support your day.
- Movement: Choose movement that restores as well as challenges.
- Stress breaks: Add short pauses during the day before your body forces one on you.
- Boundaries: Protect time, energy, and attention like they are expensive. Because they are.
- Connection: Tell someone when you are not doing well. Humans are not built to white-knuckle everything alone.
When to Get Checked Out
Even if stress seems like the obvious villain, do not assume every symptom is “just stress.” See a healthcare professional if fatigue is persistent, headaches are frequent, stomach symptoms keep recurring, sleep problems will not let up, or you are getting sick more often than usual. Get urgent care for chest pain, shortness of breath, fainting, severe dizziness, sudden confusion, black or bloody stools, or a sudden severe headache.
Real-Life Experiences: What This Can Feel Like Day to Day
The following examples are composite, true-to-life scenarios built from common experiences around stress, fatigue, poor recovery, and overload.
Jenna thought she was doing “pretty well,” which in practice meant sleeping five and a half hours, answering emails before her feet hit the floor, skipping lunch three times a week, and calling her headaches “just one of those things.” The first clue that her body wanted a slowdown was not dramatic. She simply stopped feeling like herself. She became short-tempered with coworkers she actually liked. Her neck felt tight by 10 a.m. She forgot basic tasks she normally handled with no problem. When she finally took a long weekend and slept, ate regular meals, walked outside, and stopped multitasking every waking minute, she realized how revved up she had been for months.
Marcus was sure he needed more discipline, not more rest. He added extra workouts because he felt sluggish, then wondered why his legs always felt heavy and his motivation tanked. His sleep got worse, his resting mood got grumpier, and he started needing far more caffeine to get through the workday. What helped was not “pushing through” harder. It was pulling back for two weeks, eating more consistently, replacing a few hard sessions with easy movement, and giving himself an actual bedtime. His energy did not return overnight, but it returned.
Then there is the classic caregiver story: someone handling work, family, errands, appointments, and emotional labor while insisting they are fine because everyone else seems to need them more. Often the body speaks first. Appetite changes. Stomach issues show up. Sleep becomes shallow. Joy disappears. These people are not weak. They are overloaded. And many do better once they share the load, accept help, and stop treating self-neglect like a noble personality trait.
A lot of people also notice that their body sends warning signs in layers. First comes the fatigue. Then the headaches. Then the brain fog. Then the weird overreaction to tiny things, like nearly losing it because the Wi-Fi blinked. That layering matters. It shows that slowing down does not need to wait until a full crash. Catching the early signs can save you a lot of misery later.
One of the hardest experiences to describe is the “tired but wired” feeling. You are exhausted, but your body will not fully settle. You want rest, yet your nervous system acts like you are about to give a TED Talk while being chased by bees. People experiencing this often think they need to try harder. In reality, they may need more safety cues: consistent meals, better sleep timing, fewer stimulants, less late-night scrolling, gentler workouts, and more moments of quiet that are not filled instantly by a podcast, text thread, or one more task.
The good news is that many people feel noticeably better from basic changes once they take the signals seriously. Not glamorous changes. Not expensive changes. Basic, grown-up, slightly annoying changes: more sleep, more food at regular times, less chaos, more boundaries, more recovery, and fewer attempts to prove they are secretly a machine. Your body usually does not ask for perfection. It asks for partnership. And if you listen before it starts yelling, that partnership gets much easier.
Conclusion
If your body is begging you to slow down, the goal is not to become less ambitious, less useful, or less productive. The goal is to become sustainable. Constant exhaustion, poor sleep, headaches, gut issues, brain fog, irritability, frequent illness, adrenaline surges, body aches, and loss of joy are not personality quirks. They are signals. Listen early, adjust often, and give your body enough recovery to do what it does best: keep you going without staging a revolt.